An Experimental Pelvic Congestion Syndrome Surgery Changed My Life
Key Points
- Pelvic congestion syndrome is a condition involving varicose veins in the pelvis and can be extremely painful.
- Its symptoms resemble those of premenstrual syndrome but are far more uncomfortable.
- A procedure called vein embolization is the main form of treatment, but unfortunately, the diagnosis isn't always straightforward.
When my partner rushed me to the hospital after I collapsed on the bed one night in the spring of 2021, I'd already been suffering from pelvic congestion syndrome (PCS) for some time.
I just didn't know it.
Months before, my knees buckled under me at a waterpark with my partner and kids when a sudden wave of severe pelvic pain radiated to my bladder.
Every night after the waterpark incident, I was been up most of the night in screaming pain. The symptoms resembled the worst premenstrual syndrome (PMS) of my life:
- Pelvic fullness
- Stabbing pain
- Abdominal cramps
- Radiating pelvic pain
- Lower back and bladder pain
Preliminary tests at the emergency room turned up nothing. Finally, doctors performed a CT scan of my abdomen. An hour later, an ER doctor told me there was some congestion in my ovarian veins.
"Have you ever heard of pelvic congestion syndrome?" he asked.
I hadn't.
PCS is a condition of varicose veins in the pelvis. It occurs when an internal iliac vein or ovarian vein—sometimes both—isn't working properly or has a blockage, causing venous reflux. Common in women who have given birth, venous reflux can cause severe symptoms such as pelvic or abdominal pain that worsens as the day goes on, especially with sex or exercise.
Chronic pain in women can be tricky to diagnose.
How prevalent is pelvic congestion syndrome?
More than 90 percent of women experience some symptoms of PMS, according to the Office on Women's Health (OASH). It's not always just PMS, though, as 30 percent to 40 percent of chronic pelvic pain is caused by PCS, according to a 2018 study.
PCS symptoms, such as radiating pelvic cramps and fullness, mimic symptoms of other diagnoses, such as polycystic ovary syndrome (PCOS), premenstrual dysphoric disorder (PMDD) and endometriosis.
"It's hard to find a doctor who is familiar because we don't understand pelvic congestion syndrome well as a disease and a cause for pelvic pain," said Fenwa Milhouse, M.D., a board-certified urologist, specialist in female pelvic medicine and reconstructive surgery, and the co-founder of Down There Urology in Chicago. "There is no definitive diagnostic criteria currently for PCS."
Living with pelvic congestion syndrome
It was a long path to healing for me. Armed with my CT scan results and the suggested diagnosis from the hospital, I went to my OB-GYN a few days later.
"Pelvic congestion syndrome? I'm not sure that exists," he said. "If the pain persists for another six months, we can see if it's endometriosis."
I was crushed. Living with pelvic congestion syndrome at this point was no joke. The dull aching in my pelvic area persisted 24/7, worsening to stabbing pain at night or after a long time on my feet.
There are a handful of reasons why PCS is misunderstood, ignored or disbelieved, said John Thomas, M.D., a radiologist who specializes in vascular and interventional radiology with South Texas Radiology in San Antonio. One reason is that this vascular disorder evolves slowly, so it sometimes takes a backseat to more urgent arterial diseases.
"This problem of the ovarian vein (PCS) can be annoying or even debilitating, but it is almost never life-threatening," Thomas said.
Many women with PCS don't suffer symptoms. The condition shows up frequently on CT scans, but only in certain cases—like mine—will it be the primary source of chronic pelvic pain. That's why it's so important to find a doctor who takes pain seriously.
Recommended
- Eating Dark Chocolate May Just Ease Your Menstrual Cramps: Key nutrients such as magnesium and calcium might make your PMS symptoms more bearable.
- Can CBD Relieve Period Pain?: Menstrual cramps are par for the course for many women. Cannabinoids could change that.
- Between the Pages: 'When Sex Hurts' Addresses Pain During Intercourse: Gynecologist and author Jill Krapf addresses the myths and realities of pelvic discomfort.
"Many excellent radiologists will not even mention the finding when they read a CT unless it is the only abnormality they can find," Thomas said. "I always try to at least point it out in case it is causing the patient trouble."
Current incentives in healthcare can make face-to-face time with patients scarce, which is one reason certain diagnoses get missed, said Kevin Hodnett, M.D., a family medicine specialist with Cibolo Family Medicine in Boerne, Texas.
"In medicine, we are taught to have a large list of possible diagnoses related to the constellation of symptoms that a patient presents with," Hodnett said. "Oftentimes, when physicians are pressed for time, unfortunately, this list can become more truncated, leading to missed diagnoses."
Hodnett hopes for change within the system but encourages patients to research symptoms to bring up possibilities with their physicians.
For me, it was another full year of untreated pelvic pain before I found myself in the emergency room again, unable to walk.
Finally getting answers about my pelvis pain
Same CT scan result, same diagnosis: pelvic congestion syndrome. This time, it had gotten worse.
At follow-up visits with an OB-GYN and a urogynecologist, I had to advocate for myself: I wanted ovarian vein embolization, the recommended experimental treatment for pelvic congestion syndrome. They were unsure but referred me to an interventional radiologist, who agreed.
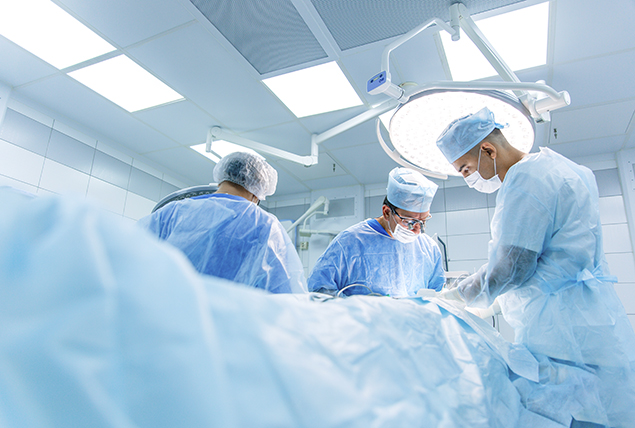
When I finally had ovarian vein embolization performed in September 2022, I felt almost immediate relief from the painful symptoms of varicose veins in my pelvis.
The procedure was low-stress, minimally invasive and performed while I was under anesthesia. The surgeon made a tiny, almost invisible incision in my neck to insert a catheter. Guided by ultrasound, they directed the catheter into my faulty ovarian vein to clot the blood and seal off the problematic vein.
My symptoms improved almost immediately. Some women, however, may feel worse temporarily before getting better. The procedure itself was so uneventful I hosted a birthday party the same evening I had it done.
Now, one year later, I am free from chronic pelvic pain. I experience virtually no PMS symptoms.
Doctors aren't always quite sure what the optimal treatment plan is for everyone with pelvic congestion syndrome, Milhouse said.
"However, embolization of the ovarian or pelvic veins has become the main form of treatment used today," she said.


















Commentary