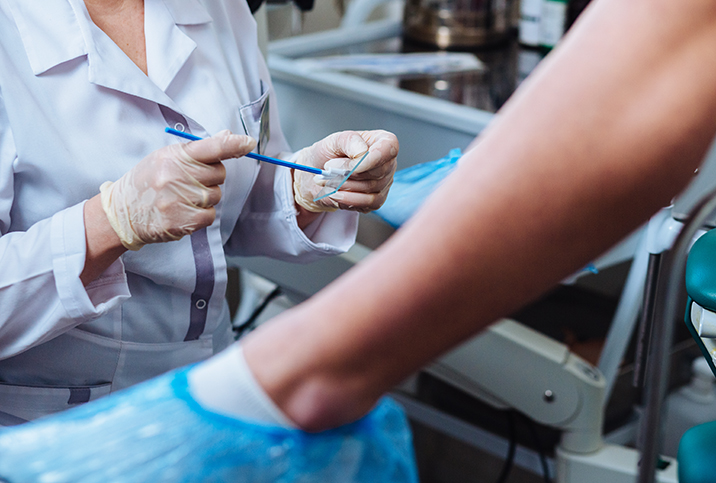
What to Expect With Cervical Cryotherapy
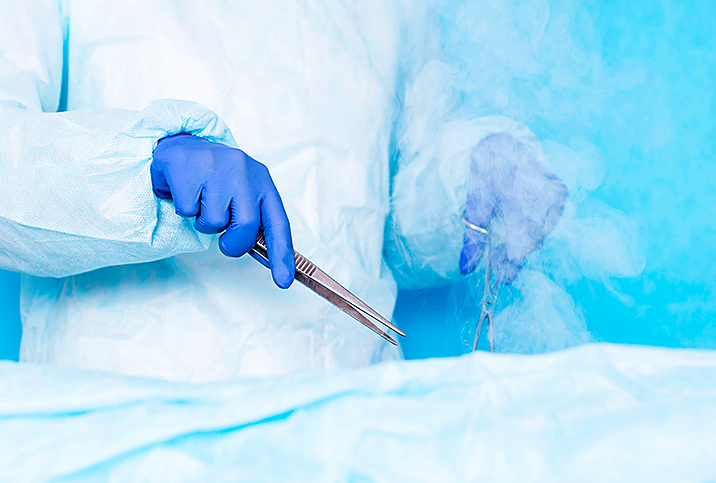
A diagnosis of "abnormal cells" following a Pap test may not mean you have cancer. But it does mean you need to schedule a follow-up with your doctor. Understanding some of your options will make the follow-up more comfortable.
One of the options is cervical cryosurgery, but let's start with some basic information about cervical cancer.
The cervix is the narrow passage that connects your vagina to your uterus. Cervical cancer—once one of the most common causes of cancer death for American women—decreased with the use of the Pap test. It was developed by George Papanicolaou, who discovered abnormal cells could be seen using a microscope to detect cervical cancer in its early and most treatable stages.
The American Cancer Society estimates about 14,100 new cases of invasive cervical cancer will be diagnosed in the United States in 2022 and about 4,280 women will die from cervical cancer. Cervical pre-cancers are diagnosed far more often than invasive cervical cancer.
Starting at age 21, women should get a Pap test every three years; more often if they've had a previous test with abnormal results.
In recent years, the HPV test has been approved as another screening test for cervical cancer. Almost all cervical cancers are caused by human papillomavirus (HPV), according to the National Cancer Institute. The HPV test looks for infection by high-risk types of HPV that are more likely to cause pre-cancers and cancers of the cervix.
Treating abnormal cells
Pap test results are usually available about a week after your appointment. An abnormal Pap smear requires follow-up care, usually starting with a colposcopy and possibly including a biopsy. Your doctor will determine if a biopsy is necessary.
During a colposcopy, your doctor will examine your cervix with a magnifying instrument used to view the extent of the abnormal cells and changes to your cervix. This exam takes place in the same office as your Pap test, and with the same routine. (Feet in the stirrups; insertion of a scapula to permit the doctor's examination.)
"Over the past 20 years, the progression of abnormality and cancer risk is better understood," said Jonathan Schaffir, M.D., a specialist in Obstetrics & Gynecology at the Ohio State University Wexner Medical Center in Columbus, Ohio. "The risk of cancer is greater with 'high grade' changes, while 'low grade' changes may go away on their own."
In some cases, with low-grade abnormal cells, ablation may be recommended. Ablation destroys the abnormal cells, which allows the body to replace them with normal cells. Two choices for ablative treatment are freezing using cryotherapy or burning using a laser or coagulation.
"Cryotherapy is safer," Schaffir said. "First, you're not exposing tissue to burning heat, and the freezing [of cryotherapy] causes less pain because it numbs the area as it's being treated."
Cryoablation carries one primary risk. "You're freezing the area, but you don't know if you've destroyed all the abnormal cells," Schaffir explained.
With low-grade abnormal cells, some cells will repair or regenerate on their own, and no ablation is actually necessary.
'Cryotherapy is safer. First, you're not exposing tissue to burning heat, and the freezing [of cryotherapy] causes less pain because it numbs the area as it's being treated.'
"Low-grade lesions are less of a worry," Schaffir said. "They are not considered precancerous."
Most doctors will recommend watching the abnormal cells for a few years. The cells will either go away or progress to higher grade abnormality that requires an excision—the cutting away of the cells and surrounding tissue for biopsy.
"Some women continue to have changes," he added. "The abnormal cells don't go away, but don't get worse. Patients who are tired of [repeated colposcopies] might get cryotherapy, but not every woman is a candidate."
The area of abnormal cells has to be the appropriate size for freezing. If the abnormal cells extend to the opening of the cervix, cryotherapy is not recommended.
If cryotherapy is chosen, the most common side effects include cramping and a "copious watery discharge" following the procedure. Ibuprofen is recommended for cramping. The discharge will last for about a week, as the cervix heals.
"It requires consistent pad use," Schaffir said. Intercourse is not recommended for two to three weeks, but there are no long-term negative effects.
What other options should be considered?
Valerie Busick, M.D., an obstetrician and gynecologist with Avina Women's Health in Central Ohio doesn't perform cryosurgery.
"I treat cervical dysplasia with a cautery procedure called LEEP [Loop Electrode Excision Procedure]," she said. With LEEP, a tissue sample can be sent to the lab, which can't happen with cryotherapy. She has several older patients who had cryotherapy years ago.
The biggest concern with either cryotherapy or laser ablation was the inability to confirm the removal of all abnormal cells.
"There was no specimen," Busick explained. "With LEEP, pathology can take a closer look and I'm ablating the cells."
"Cryosurgery is still an option for treating cervical dysplasia, but it is falling out of favor due to the ease of LEEP," added Jason Melillo, M.D., a specialist in obstetrics and gynecology and vice president at Ohio Health.
What questions should you ask your doctor?
If you've learned that you have abnormal cervical cells, there is one question you should ask: Is treatment necessary? A mild abnormality may clear up on its own. A follow-up to determine the grade of abnormality is the first step, and a colposcopy can help determine if treatment or biopsy is necessary.
Like Busick and Melillo, Schaffir rarely recommends cryotherapy. In addition to other alternative treatments, he notes one important factor: There is less cervical cancer now.
"Gardasil—the vaccine for HPV—has made a big difference," he said.