Know What Can Interfere With Your Birth Control
Ancient Egyptians invented condoms 3,000 years ago. We don't know what they were made of—maybe animal hides—but the ancients were depicted in pictures as having wrapped it up. We know people were continuing to think about contraceptives because 1,200 years later, in 1250 BC, they created pessaries, a vaginally inserted contraceptive used to kill or block sperm. These pessaries were made from crocodile dung, sodium carbonate and honey.
It wasn't until 1844 that rubber condoms were created (meant to be washed and reused, of course). George Bernard Shaw, the playwright, called them "the greatest invention of the nineteenth century."
Let's be thankful that progress has continued, and we now have a plethora of safe and effective birth control options. Still, they aren't 100 percent effective 100 percent of the time. Things happen. And because things happen, it's important to know why and how they do, so we can, hopefully, avoid them.
Birth control options
Monica Grover, D.O., head gynecologist at VSPOT sexual health spa, identified the most common forms of birth control used today. "There are five classifications for contraception that require different methods of administration or application," she said. "The most common is the long-acting and short-acting hormonal contraceptives, as well as barrier contraceptives."
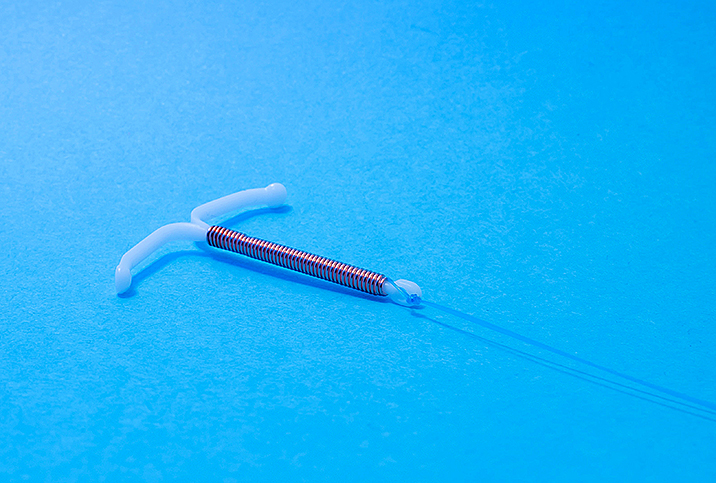
Long-acting hormonal contraceptives are 99 percent effective against unwanted pregnancies. These are generally options such as intrauterine devices (IUDs) or the Nexplanon arm implant. Unlike other forms of birth control, these don't require the patient to do anything beyond attending the appointment to get either device implanted—and they last anywhere from 3 to 12 years.
IUDs are a great option for patients who don't want to worry about their birth control daily. "Long-acting IUDs are the best options for women who may want children in the future," Grover said. "Once implanted, they should not be noticeable and can be removed whenever the patient decides they are ready to start trying for pregnancy."
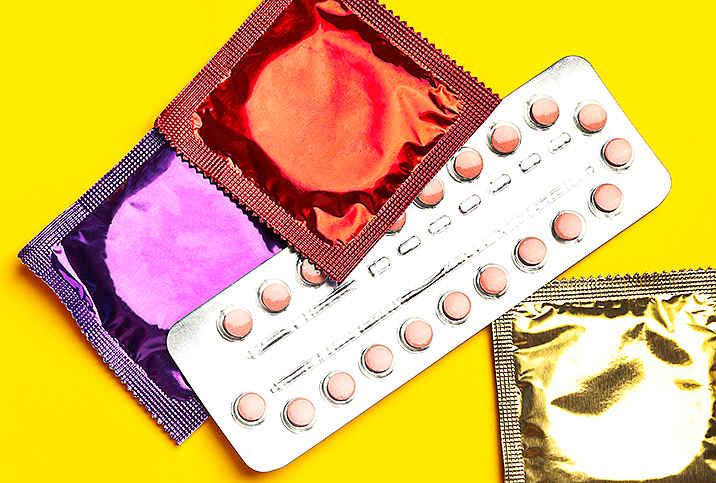
Short-acting contraceptives are things we associate more with nonsurgical options, such as pills, patches, shots and rings, that must be used regularly as instructed in order to retain their high efficacy rates. (The key phrase is "as instructed.") When misused or used with irregularity, the efficacy of these forms of birth control is highly compromised.
Barrier contraceptives—condoms, diaphragms and cervical caps—have an efficacy of around 70 percent to 88 percent.
What this means is that couples utilizing short-acting birth control methods, barrier birth control or a combination of the two need to be meticulous about consistently using their birth control as prescribed and instructed. When referring to things that can interfere with birth control, the first thing we have to acknowledge is inconsistency.
Of course, that's not the only factor that impacts birth control efficacy.
What can make my birth control not work?
"Because [certain birth control] medications are taken by mouth, they rely on the intestinal absorption to enter the body," said Betsy Greenleaf, D.O., a board-certified urogynecologist. "We don't often think of the health of our intestines, however gut health is becoming a hot topic as of late. Inflammatory foods, such as sugar, gluten, dairy and processed foods, can wreak havoc on our intestines, leading to gut inflammation that can affect the absorption of nutrients and medications, such as birth control."
Not only can inflammatory foods cause issues with birth control—and other orally ingested medications—but so can certain other drugs. Especially, as Greenleaf pointed out, ones that affect the liver or compete for the same receptors as birth control medications. Both she and Grover pointed out that medications used to treat HIV, fungal infections, seizures and some antibiotics can disrupt the efficacy of oral birth control medications.
Greenleaf also mentioned that some IUDs rely on the liver to process hormones, meaning they too can be affected by other medications, supplements and foods that affect the liver. Copper IUDs, however, don't involve hormones at all.
And while common issues with barrier birth control, such as condoms ripping, drying out or expiring, might come to mind easily, there are also lesser-known variables at play with nonmedication or surgical birth control.
For example, Greenleaf acknowledged that some people prefer to use what they believe to be natural lubricants—things such as coconut oil or massage oil—but given that most condoms used now are made of latex, this is actually detrimental to the security a condom would provide. Oils wear down latex, and even some petroleum-based substances will, as well.
In other words, if it isn't lube, don't use it as lube.
How can I be sure my birth control is working?
First things first: Always talk to your doctor about the pills and medications you are taking. Your physician will be able to inform you of any medication interactions that can decrease the efficacy of your birth control. If you're anxious at all (aren't we all?), schedule an appointment.
Birth control pills work best if taken as instructed. Miss one pill? Take it as soon as you remember. Miss multiple pills, go ahead and use a backup contraceptive, such as condoms, or avoid sex until you've taken your birth control pills for a full seven days.
If your preference is condoms, take the time to ensure the condom is not expired or ripped. And check your lubricant to make sure it works with latex. Usually, water-based or silicone-based lubes are best.
Whatever type of contraceptive you use, there are factors that can decrease the efficacy. So be careful, follow the instructions and talk to your doctor about any concerns. And regardless, I think we can all be thankful we're not coating our private areas in crocodile dung anymore.