The Limitations of Prenatal Genetic Testing
Editor's Note: On April 19, 2022, the FDA issued a bulletin warning the public about the risk of false results, inappropriate use and inappropriate interpretation of results with non-invasive prenatal screening.
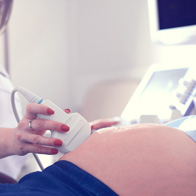
Prenatal genetic screening for birth defects has advanced by leaps and bounds since ultrasounds were first developed in the 1950s. The most current, cutting-edge crop of screening tests attempts to detect chromosomal abnormalities in a fetus by looking for microdeletions or microduplications in chromosomes through an analysis of the mother's blood.
These tests were the focus of a recent New York Times investigation, which determined many of them often deliver false-positives to patients; in other words, warning of a disorder when it doesn't exist. Here's a look at what prenatal genetic testing can—and can't—tell people about their pregnancies.
Understanding prenatal genetic testing
Patients may undergo a battery of different tests during pregnancy, depending on maternal age, individual risk factors, physician recommendations and personal choice. Prenatal testing falls into one of two categories: screening tests and diagnostic tests.
"Prenatal tests allow parents the opportunity to readily identify issues in a timely manner, such that they can make a determination to maintain a pregnancy or terminate a pregnancy based on the findings," said Kecia Gaither, M.D., M.P.H., a board-certified OB-GYN and director of perinatal services at NYC Health + Hospitals/Lincoln in the Bronx in New York City.
Screening tests are noninvasive and include ultrasounds and maternal blood tests. They can also tell you the chances that your fetus will have certain genetic disorders, according to the American College of Obstetricians and Gynecologists (ACOG). Screenings assess risk; they do not definitively diagnose conditions.
Older blood tests, such as the quad screen, are still administered, but cell-free DNA (cfDNA) screenings have grown in popularity since they became available to patients in 2011. These tests analyze fetal DNA from the placenta and evaluate the risk of fetal aneuploidy, which occurs when the baby has missing or extra chromosomes, including trisomy 21 (Down syndrome) or Turner syndrome. They can be done in the first trimester and can also tell expectant parents the sex of the baby weeks before an ultrasound, though not always accurately.
Diagnostic tests are typically conducted after a patient has received a positive result of an abnormality from a screening test. Amniocentesis and chorionic villus sampling (CVS) are the two primary diagnostic tests. Both are invasive, using a needle to extract either a sample of amniotic fluid or placenta to examine fetal cells.
As screening tests have become more sophisticated and accurate—particularly cfDNA for Down syndrome—these diagnostic procedures are performed far less frequently. Both CVS and amniocentesis have a risk of procedure-related miscarriage. But these tests confirm screening results and help guide the recommended follow-up after a positive screening.
"We still do amniocentesis and chorionic villus sampling," said Angie Jelin, M.D., a prenatal geneticist, associate professor and director of the first trimester screening program at Johns Hopkins Medicine in Baltimore. "Those are actually taking fetal tissue and testing it. If you really want a concrete outcome, that is the test you want."
The false-positive problem
Cell-free DNA screenings can accurately detect Down syndrome (1 in 700 births) 99 percent of the time, Jelin said. But these screenings are less accurate for other rarer and usually fatal genetic conditions.
False-positives from several screening tests were the center of the Times investigation. Positive results from microdeletion screenings for DiGeorge syndrome (1 in 4,000 births) were incorrect 81 percent of the time. For Prader-Willi and Angelman syndromes (1 in 20,000 births), the tests delivered false-positives 93 percent of the time.
"We know the technology is advancing and getting better," Jelin said. "It's just that currently, these conditions are so rare that you need a very high sensitivity and specificity in order to not have a lot of false-positives."
Jelin said Johns Hopkins does not recommend patients have microdeletion testing done, because these tests are not as sensitive or specific as they could be and the conditions they're screening for are so rare.
What pregnant patients need to know
ACOG guidance states screening and diagnostic testing options should be discussed and offered to all pregnant patients regardless of maternal age or risk of chromosomal abnormality.
It's this discussion between patients and OB-GYNs or genetic counselors that's critical.
"Patients need to know what test they're having, they need to know why they're having it and they need to know that it's a screening test," Jelin said.
Patients also need clear guidance on next steps should they receive a positive result.
Currently, no "umbrella" test exists to screen for every chromosomal abnormality at once, Jelin said. But it's coming. While noninvasive prenatal whole genome sequencing is not available to patients, it has been demonstrated in a lab, according to 2019 research from the National Institutes of Health's National Human Genome Research Institute.
As more genetic information about their baby becomes available to expectant parents, demand will grow for genetic counselors and OB-GYNs who can accurately interpret and clearly explain the results—and recommend next steps. There were 2,400 genetic counselor jobs nationwide in 2020, but that number is expected to increase 26 percent by 2030, according to the U.S. Bureau of Labor Statistics.
A decision on testing comes down to understanding risk—and the distinction between screening and diagnostic tests.
"Patients need to understand the difference between a test utilized for screening for a genetic abnormality versus a test being utilized definitively for diagnostic purposes, actually diagnosing a genetic abnormality," Gaither said.