A Guide to Getting Your First IUD
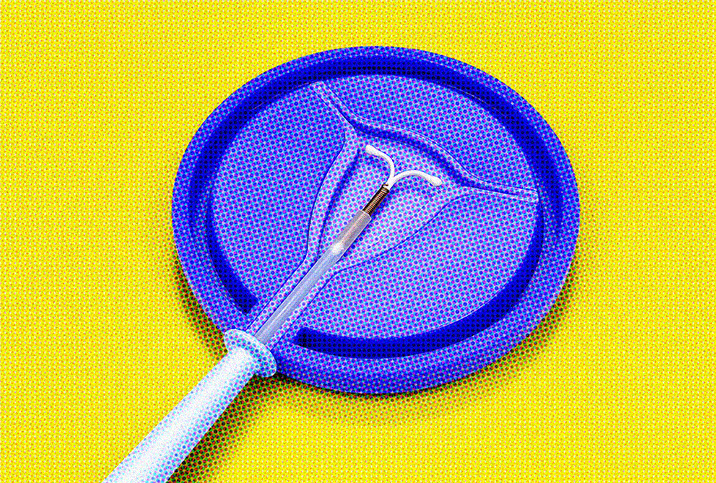
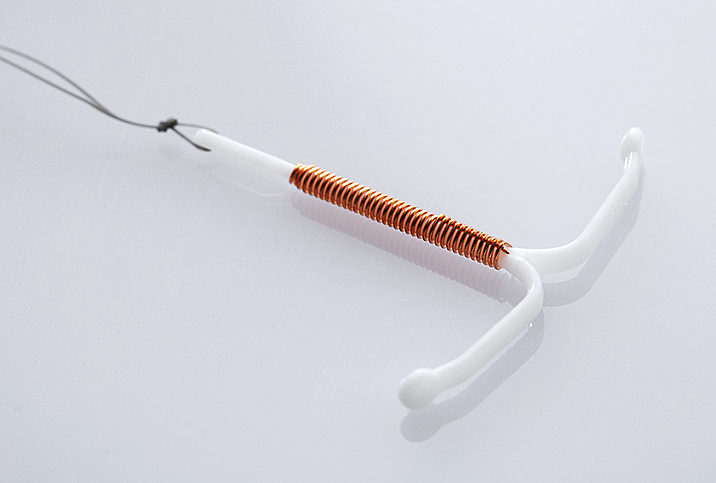
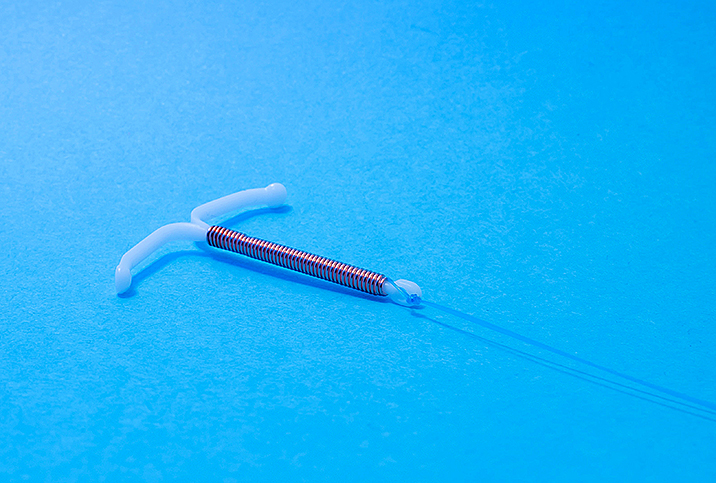
An intrauterine device (IUD) is a small T-shaped contraceptive implement inserted by a trained professional into a woman's uterus to prevent pregnancy. The two basic types work in different ways, and your gynecologist will discuss which is best for you.
Hormonal IUDs release progestin, which increases cervical mucus that can trap sperm, sometimes prevents the release of an egg from the ovaries, and thins the lining of the uterus to make it difficult for a fertilized egg to implant there. The nonhormonal copper IUD prevents sperm from moving around to meet with the egg. Its copper molecules are spermicidal, and it also sets up a local inflammatory response that interferes with fertilization and implantation.
IUDs work for five to 12 years, depending on the type, and can be inserted at any point during a woman's menstrual cycle. It is preferable to insert an IUD when a woman is on her period, since the cervix is open and there's no chance that pregnancy occurred prior to insertion. They can also typically be placed after a woman gives birth or after an abortion.
If circumstances change, women are physically able to get pregnant right away once their IUD is removed. IUDs are covered by many health insurance plans, including Medicaid and other governmental programs.
Preparation
Continue with your current birth control methods until your IUD is placed. You may want to wear something comfortable like loose-fitting pants in case you have cramping after the procedure, and bring a pad in case there is any spotting or bleeding. If you're worried about discomfort, some clinicians prescribe a medication to help loosen or numb the cervix prior to the procedure. And many providers recommend taking ibuprofen 30 minutes before insertion to decrease cramping.
What to expect
After cleaning your vagina and cervix with an antiseptic, the doctor or nurse will use a special insert to place the IUD into the base of your uterus. The string on the IUD will be trimmed so only a few centimeters hang out of your cervix. The procedure is quick—typically only five to 15 minutes—and any cramping usually subsides. Eat a snack beforehand to reduce the risk of getting dizzy or lightheaded, and it's a good idea to have someone go with you to drive you home.
Afterward
Make a note of when you got your IUD so you'll know exactly when it needs to be replaced.
You may want to take the day off from work or other obligations so you can go home and get comfortable after the IUD insertion. Discomfort, cramping, bleeding and spotting are common, but these effects typically discontinue in three to six months, if not sooner. Over-the-counter pain meds will help, as well as a heating pad or a heated water bottle on your abdomen. Most people resume normal activities the next day.
Don't insert anything into your vagina for 24 hours after the procedure. After a day, you can have sex again, but doctors can't guarantee that either type of IUD will be immediately effective, so it's highly recommended you use backup protection, such as condoms, for the first two weeks.
Hormonal IUDs often make menstrual periods lighter or shorter. Some women stop getting them entirely, which is also normal. Hormonal IUDs can decrease cramps and reduce PMS, endometriosis and polycystic ovary syndrome (PCOS) symptoms. The copper IUD can cause increased bleeding and cramping with your period, especially within six months of its insertion.
In rare instances, IUDs can become displaced or fall out. You can check on their placement by inserting clean fingers into the vagina and gently feeling for the string. Don't pull on it. If you can't feel it, call your doctor immediately. Displacement is most common early on, so you should see your clinician one to two months after insertion to confirm your IUD is in place. It can be removed if you want to try to conceive or switch birth control methods. You should contact your physician if you think you might be pregnant or if you have extremely heavy bleeding, sharp pains in your abdomen or pelvis, pain during sex, chills or a fever over 101 degrees, or foul-smelling discharge from your vagina.
A lot of women are nervous before they get their first IUD. In reality, it's very similar to a Pap smear: a little temporary discomfort and then you're done. The freedom of worry-free, long-term birth control is worth it.