'Bag of Worms' Below the Belt? You Have Intervention Options
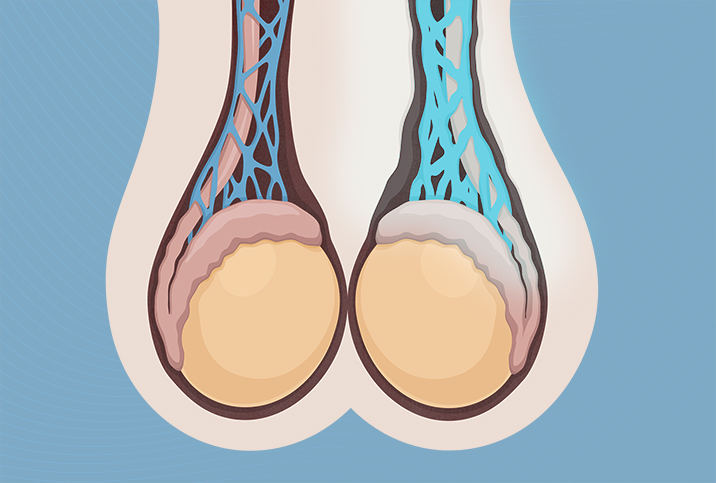
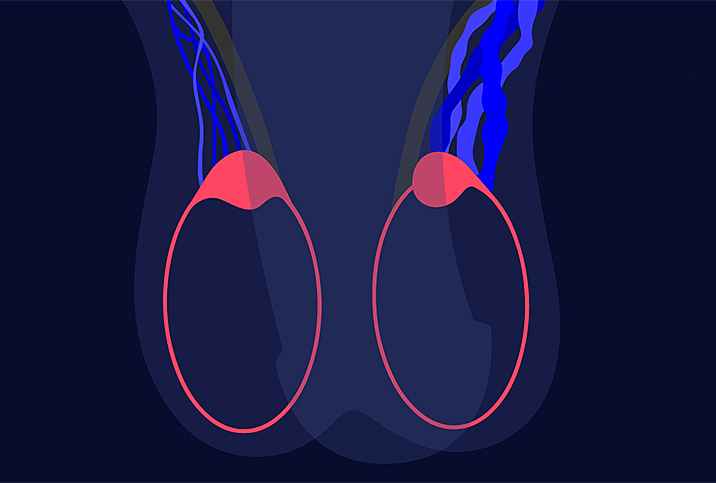
Most of the 15 percent of adult males who develop varicoceles—a chronic dilation of the veins that drain blood from the testicles—experience no threat to their overall health and are often treated with a simple wait-and-see approach. However, varicoceles can affect quality of life or fertility for some men, particularly in more advanced cases.
Varicoceles are the number-one cause of correctable male infertility, according to Robert P. Caruso, M.D., a urologist and robotic surgeon at Clara Maass Medical Center in Belleville, New Jersey. He explained the varicoceles-caused dilation eventually increases the temperature in the testicles, which can impact sperm production and impair fertility.
Adam Ramin, M.D., a urologist and the medical director of Urology Cancer Specialists in Los Angeles, added that varicoceles can be unsightly and upsetting to some individuals.
"It causes a typical appearance of what we call a 'bag of worms,'" he noted. "So people with varicoceles look like they have a bunch of worms inside their scrotum next to their testicles."
Some patients develop achiness or pain in their testicles, and varicoceles may lead to atrophy, meaning the testicles get smaller over time, according to Ramin.
Options to treat varicoceles are important for any man who wants to conceive with a partner, anyone experiencing significant pain or distress over their "bag of worms," or someone who is suffering additional side effects. Explore these five options.
Monitoring
Caruso noted the exact treatment for varicoceles starts with grading. Typically, cases of grade 2 or higher are eligible for treatment, while grade 1 varicoceles that aren't affecting a patient's quality of life require a monitoring approach for treatment.
At grade 1, the dilated veins can be felt by a urologist conducting a medical exam when the patient is bearing down or straining.
"If the varicocele is grade 1 and is not resulting in infertility, then treatment is probably not needed, but the patient and his doctor should keep an eye on it," Caruso added.
Surgery
A man with varicoceles more severe than grade 1 may be eligible for surgical repair, which involves getting inside the testicles to physically close off the dilated veins. At grade 2, the dilation can be felt by a urologist during an exam with the patient standing, even without straining. At grade 3, the dilated veins are clearly visible through the skin.
"Typically, for grade 2 or higher, if the varicocele is impacting fertility, then that patient would be a candidate for repair," Caruso said.
A semen analysis can detect abnormalities, such as decreased sperm count or issues with the appearance and movement of the sperm, which could indicate fertility has been impaired.
Ramin explained that if the patient's primary motivation to get surgery is because of pain in the testicles, it's important to have a conversation with the doctor because, unfortunately, surgery doesn't always take away the pain.
Microsurgery
While different types of surgery can treat varicoceles, Caruso said the "gold standard" is microscopic subinguinal varicocelectomy, also called microsurgery.
There are two approaches to microscopic varicocelectomy surgery: subinguinal, which Caruso mentioned, and inguinal. During the latter procedure, an incision is made higher in the groin so the surgeon can access the ilioinguinal nerve and snip it, which should relieve the pain. For subinguinal surgery, which is the most common kind, the incision is made lower in the groin—just above the scrotum, Caruso said—to access the enlarged veins and tie them off, limiting unwanted blood flow.
Surgeons use a microscope to avoid lymphatic vessels and otherwise ensure they keep essential structures intact.
"Because it is a small and less invasive procedure, it involves a quick recovery and there is generally not much pain associated with it," Caruso explained. "Although there are also more invasive surgery options, using the small incision and the operative microscope has become the standard."
Embolization
Embolization involves an interventional radiologist using imaging to place a catheter to divert blood away from the varicocele.
This procedure requires a tiny groin incision and can be especially helpful for the small percentage of patients who have a recurrent varicocele after previous repair.
Caruso explained that embolization is typically reserved as a secondary treatment—subinguinal varicocelectomy is the first choice—because the procedure carries the potential for vascular risks.
Helpful actions at home
While no "home remedies" exist for varicoceles, men may be able to ease the physical effects of varicoceles with some measures, such as switching from boxers to briefs.
"In many instances, that helps with the pain," Ramin said. "Especially if they're playing sports, it would be important to wear some support so the testicles are less like hanging down and more supported."
Men can also make time to lie down to allow blood flow back toward the heart and take anti-inflammatory medications, such as ibuprofen, to help with the pain.
It's important for men with varicoceles to keep in communication with their doctor and notify them if they experience any change in their symptoms.
Caruso also pointed out that different life factors, physical traits, lifestyle choices and employment can affect how varicoceles may need to be treated. For example, pain can increase with straining or physical activity, or lead to further effects that would require repair.
It's important for men with varicoceles to keep in communication with their doctor and notify them if they experience any change in their symptoms—even if you don't need treatment now, you may need it later.
"Generally speaking, the more severe or the more dilated the veins are, the more likely it is that a patient would need a treatment because the more likely it is that they have infertility or they might have atrophy of their testicles," Ramin said.
Fortunately, any type of varicocele is never an emergency or urgent condition—it's not life-threatening—and there may be an appropriate treatment for you.