Symptoms and Diagnosis of Syphilis

Syphilis is a sexually transmitted disease (STD) that, if untreated, can wreak devastating damage to a body.
Prior to the development of antibiotics in 1910, syphilis ravaged nations around the world in plague-level proportions. More than a century later, modern medicine had developed screening as well as diagnostic and treatment methods to help diminish the impact of syphilis to the point that it was no longer regarded as a threat.
Over the past decade, though, it seems as though syphilis may be making a comeback.
The many stages of syphilis
Today, the majority of syphilis cases are documented among gay, bisexual and other men who have sex with men. Men in general account for more cases of syphilis than do women, with minority and lower-income communities disproportionately impacted at higher levels. This, in part, has been theorized to be due to a lack of sexual education and less access to quality healthcare.
Syphilis cases among women who primarily have sex with women have also shown marginal increases over recent years.
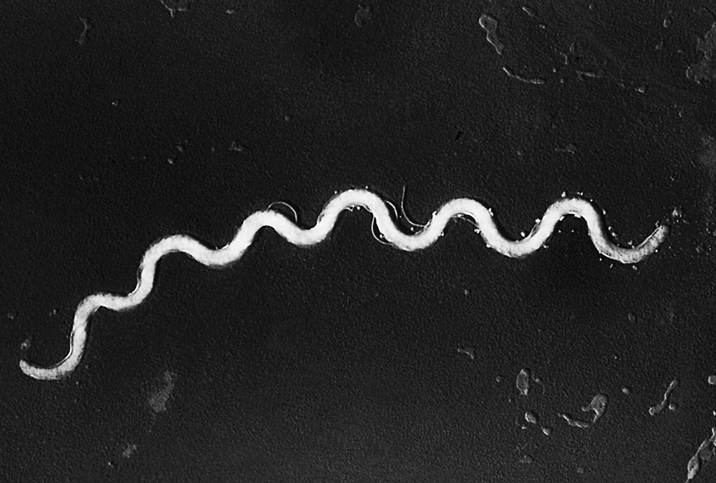
Syphilis is contracted through intimate contact, which creates an opportunity for exposure to and transmission of Treponema pallidum bacteria. The condition manifests in the form of different stages, each associated with specific symptoms.
The stages of syphilis can overlap; they can also progress forward or regress to previous stages. With the advances in modern medicine, the latter stages of syphilis are now less common. The first three stages, however, continue to be the most prevalent ones experienced by those who contract the disease.
Syphilis earned the moniker "The Great Imitator" because some of the early symptoms are similar to a large number of other diseases. This is one reason why getting regularly tested for STDs (especially when you have multiple partners or are in a relationship with someone who has multiple partners) is important, as you may never suspect that the cause of your ailment is syphilis.
Following are the many stages of syphilis.
The primary stage
The primary stage of syphilis is most notably marked by the appearance of a single chancre, or ulcer, although more than one can be present on the body at the time of diagnosis. A chancre is a unique sore, usually round and firm, and is typically painless.
The primary chancre forms at the point of entry of syphilis into the body, which may be in a hard-to-notice location, such as the genitals or anus. Whether you're aware of the chancre or not, it will appear for three to six weeks, and then it will heal as if it were never there.
During the primary stage, syphilis is contagious and you will likely transmit the disease to any sexual partners during this period.
If the chancre was undetected and untreated, syphilis will enter into its secondary stage.
The secondary stage
The secondary stage of syphilis is closely associated with rashes and the development of mucous-membrane lesions in areas like the mouth, vagina or anus.
It's typical for syphilis-related rashes to form in the same area as the primary chancre, at which point they might be faint in color, but are unlikely to cause any discomfort or itchiness. It's also possible for secondary stage syphilis to be characterized by a spread of spotty red or reddish-brown rashes on the palms of the hands or soles of the feet, though these rashes can appear elsewhere on the body, too.
Secondary stage rashes may not develop until several weeks after the primary chancre has healed post-infection.
A number of other symptoms are also associated with this stage of the disease, including fever, swollen glands, hair loss, weight loss, muscle aches, fatigue, headaches, sore throat and lesions.
Secondary stage syphilis will heal eventually with or without treatment, and all symptoms will seem to have disappeared. However, the absence of symptoms does not mean syphilis is no longer present or contagious.
The latent stage
The latent stage of syphilis is often referred to as the "hidden" stage of syphilis because no visible symptoms are present, and it may seem as though whatever symptoms you may have experienced are now gone and the condition is healed.
Latent stage syphilis is broken into two categories: "Early" latent-stage syphilis means the condition has progressed to this point within 12 months of exposure, whereas "late" latent-stage syphilis refers to syphilis that reaches this stage more than a year after exposure.
Syphilis is still alive and well in your system during the latent stage, and you are contagious even if you are experiencing no symptoms. Latent syphilis can last for many years, so without regular and consistent testing practices, you can unknowingly pass the disease on to many sexual partners.
It should be noted that while there are specific symptoms for each stage of syphilis, this disease can attack and damage various parts of the body—like the nervous system, eyes or lungs—at any time. The likelihood of experiencing any of these symptoms will depend on your unique health history and biology.
The tertiary stage
With modern treatments and screening options now available, tertiary syphilis is much less common.
Tertiary syphilis can develop as many as 10 to 30 years after the initial infection, and its effects can be fatal as it often targets a number of vital organs. Complications can arise in the bones, blood, joints, heart, nerves, brain, eyes, muscles, lungs and liver.
In this stage of syphilis, the infection is not contagious.
Neurosyphilis, cardiovascular syphilis and ocular syphilis
These conditions describe specific instances of syphilis in which particular parts of the body are uniquely and dramatically impacted.
Development of these focused versions of syphilis typically results from the absence of treatment and can lead to brain damage, permanent breathing issues and blindness.
Congenital syphilis
Congenital syphilis is less common than the three main stages of syphilis, but medical professionals are concerned about the rising numbers of cases around the country.
Congenital syphilis is syphilis passed from mother to child during pregnancy and/or the birthing process. A range of complications can result from a case of fetal or infant syphilis, and the likelihood of a mother passing the STD to her child is increased if the mother has a long history of the disease.
If the baby contracts syphilis, potential results may include premature birth, various birth defects, brain damage, miscarriage, stillbirth or death shortly after birth.
All pregnant women should be tested for syphilis; most doctors will include the test at the first prenatal appointment. If syphilis exposure risk is high for a woman who is pregnant, multiple tests throughout pregnancy may be recommended.
Diagnosing syphilis
Two types of blood tests are primarily used to identify and confirm a syphilis diagnosis:
- Nontreponemal tests
These are the more simplistic of the two types of blood tests used for syphilis screening. Nontreponemal tests are considered useful for screening, but a reactive result requires further confirmation via treponemal testing. Without secondary validation, nontreponemal tests can be considered inaccurate or susceptible to false positives. - Treponemal tests
Treponemal tests are used in conjunction with nontreponemal tests to confirm a syphilis diagnosis. These tests identify antibodies specific to syphilis, which can be found even long after the successful treatment of the disease.
It is also possible to diagnose syphilis by identifying the presence of Treponema pallidum bacteria using dark-field microscopy. This technique is rarely used as blood testing falls more in line with procedural practices for most care centers, hospitals and doctor's offices today.
Beyond diagnosis
Syphilis is fairly easy to treat in the early stages with antibiotics, but due to the potentially discrete presence of syphilis—especially during the latent stage—regular testing is important.
If you've received a positive syphilis diagnosis, follow your doctor's instructions and cease all sexual activity. Your recent sexual partner or partners should also be notified if there is even the slightest chance of their exposure, or if they were potentially the person who transmitted the illness to you.
Because syphilis diagnoses are associated strongly with a higher risk for HIV, ongoing HIV testing should also be a priority. Sores caused by syphilis increase the odds of contracting HIV upon exposure, and the presence of syphilis is estimated to increase the chances of contracting HIV by as much as two to five times upon exposure.
Penicillin is highly effective for fighting syphilis, but there are options—such as penicillin desensitization treatment—for those with penicillin allergies.
Syphilis is extremely dangerous to you and your sexual partners if untreated. If you are sexually active, it's important to get tested regularly and follow the advice of your doctor.