Sometimes, Radiation for Prostate Cancer Is the Best Option
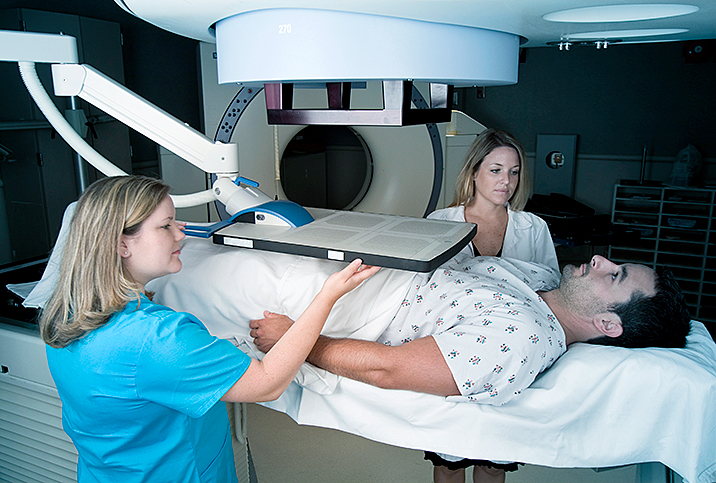
When you begin researching prostate cancer, you quickly learn there's no one-size-fits-all answer or approach to treatment. Each patient has unique circumstances and goals around which healthcare teams try their best to craft personalized care strategies.
But the two main silos most interventions fall under are prostatectomy to surgically remove the prostate gland and radiation therapy to attack the cancer while leaving the prostate gland in place.
Several factors go into choosing one treatment over the other, including the patient's age, health and long-term goals, and the aggressiveness and risk level of their particular cancer.
The right choice for the patient
It's essential to note that extensive studies show both prostate radiation therapy and prostatectomy are fine choices, and neither has a clear advantage over the other in terms of effectiveness.
"Both radiation and surgery are very effective," said Peter Reisz, M.D., a urologic oncologist with Lehigh Valley Health Network Urology in Pennsylvania. "We're lucky we have two great tools. But I do want to say radiation is quite well-tolerated these days with the modern technology that our radiation oncology colleagues have."
Age
Age is a crucial factor in choosing between prostatectomy and radiation therapy for a number of reasons that aren't always obvious.
For older patients, the increased frailty of the body's systems may point toward radiation therapy over surgery.
"Older patients into their 70s and even 80s have been shown to have more and worse side effects after surgery in terms of urinary leakage and erectile dysfunction, so that would also push us toward radiation in some cases," Reisz said. "The men who recover best after surgery are those who have no issues before the surgery, so those men tend to be younger."
Another common side effect of both kinds of prostate cancer treatment is erectile dysfunction (ED). However, there are important differences in how men commonly experience ED following surgery versus radiation, and age is a definite factor.
Surgery may affect the nerves that govern erections, causing immediate effects on the patient's erectile function. Over time, however, and with modern nerve-sparing surgical techniques, most patients can recover functional erections with the help of medication.
Radiation therapy can also damage those nerves, but any damage takes time to set in. Patients usually experience no immediate effect on erectile function in the first few years after treatment; eventually, however, erectile function can decline. Studies show that after about 15 years, the rates for ED are about the same for men who have undergone either prostatectomy or radiation therapy.
"A young man in their 40s or 50s may care a great deal about their erectile function, whereas a man in his 80s may not," Reisz said. "So we generally recommend surgery for younger men because they have a much longer time course."
Overall health
While prostatectomy techniques have advanced greatly in recent decades, surgery is still stressful on the body. The health of the patient can influence the decision-making process.
"People come in with different medical histories," Reisz explained. "Someone who is very, very sick or has heart problems may be too sick to undergo a surgical procedure, so we may recommend them for radiation."
Low-grade and localized
Radiation is often the first treatment choice for patients who have low-grade cancer that is localized in the prostate, according to the American Cancer Society, and the rates of recovery for men with this type of cancer are about the same as those who have a radical prostatectomy.
Metastasized
Interestingly, it's the other end of the scale where radiation again may become the more recommended option. For patients who have cancer that has spread outside the prostate to other organs or tissue, surgery is usually off the table due to the difficulty of removing the cancer in its entirety.
There is some data to suggest that treatment of the primary cancer may have some benefit even in metastatic disease. The STAMPEDE trial, arm H, demonstrated a survival benefit for newly diagnosed prostate cancer patients with low metastatic burden who additionally received radiotherapy (RT) to the primary.
Personal preference
Some patients may have a strong preference for one treatment approach over the other for various reasons, such as an aversion to surgery or to give themselves a better shot at retaining erectile function in the short term.
Modern radiation therapy techniques specific to prostate cancer are streamlined procedures and precision-targeted so they can minimize damage to surrounding tissue.
"A lot of guys, when they're diagnosed, they choose to have what's called curative or definitive radiation, not surgery," said Daniel E. Spratt, M.D., the Vincent K. Smith chair in radiation oncology at University Hospitals Seidman Cancer Center in Cleveland. "That's increasingly in use, especially now that we're often using just five treatments of radiation rather than the old 40 or 45 treatments. There's less chance for incontinence or urinary leakage, and there's a lower chance for erectile dysfunction."
Other considerations
Keep in mind that providers often recommend androgen deprivation therapy (ADT), sometimes called hormone therapy, in combination with radiation therapy. It is very effective but can have dramatic side effects because it basically wipes out the body's testosterone production. Those repercussions may include hot flashes, bone degradation, loss of muscle mass, ED, low libido and more.
In the short term, radiation therapy causes inflammation in the tissue surrounding the prostate, which brings the bladder and the rectum into the picture. Patients might experience burning when they urinate, blood in the urine, diarrhea, burning with bowel movements or rectal bleeding, all of which are normal for a few weeks after completing treatment.
But further down the line, a small percentage of men may experience similar, yet graver, effects.
"In the long term, some patients can develop a sort of a scarring in the bladder or rectum, and that can cause bleeding from the bladder or even defunctionalize the bladder, where it doesn't work very well," Reisz explained. "It can also cause scarring in the urethra itself, preventing them from urinating normally. That's a small percentage, but there is a risk. It's called radiation cystitis."
Last, a small percentage of patients—fewer than 2 percent—may develop a secondary cancer in the bladder or rectum due to their radiation exposure. This can take 10 or 20 years to develop.
Conclusions concerning radiation for prostate cancer
Any treatment for any cancer is likely to have secondary effects on the body. However, modern techniques and the precision with which radiation oncologists wield them have made radiation for prostate cancer one of the safest, most effective cancer treatments.
"It is very targeted at the prostate, not nearly like it was even 10 years ago," Reisz said. "So the incidence of true, severe problems is pretty low."