The Facts About Prostate Exams
Located below the urinary bladder and in front of the rectum, the prostate is a gland found only in men. The prostate produces fluid that is part of semen and helps move the semen through the urethra during ejaculation. This gland is also susceptible to irregularities, chronic conditions and cancer.
Prostate cancer is the second most common form of cancer for men in the United States. According to the American Cancer Society, in 2020 there were an estimated 191,130 new cases of the disease and 33,330 associated deaths. Fortunately, if detected early, prostate cancer is highly treatable, and most men survive the diagnosis, with more than 3 million prostate cancer survivors alive today in the U.S. as proof. Prostate cancer is often asymptomatic—there are no visible signs or symptoms until the disease is in its advanced stages—so screening is essential to making an early diagnosis.
Cancer screening is an important function of prostate exams, but that is not all they are used for. Prostate screening can also detect conditions like prostatitis or benign prostatic hyperplasia (BPH). Compared to prostate cancer, men will likely feel the effects of these conditions before they're tested, but a thorough screening will be able to discern the likely problem and lead a doctor to the best possible treatment plan.
Types of exams
Prostate exams include the digital rectal exam (DRE) and the prostate-specific antigen (PSA) test. You don't have to do anything to prepare for either of these screenings.
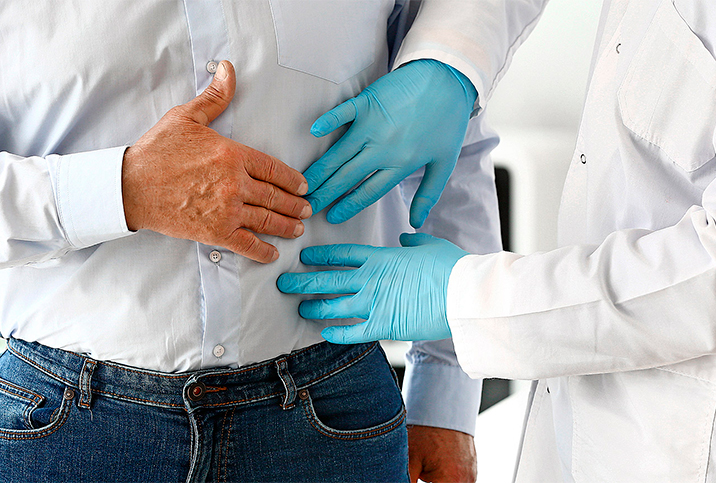
During the DRE, the doctor will insert a gloved and lubricated finger into the rectum to physically feel the prostate. Here, they'll estimate the prostate gland's size and feel for nodules, hard spots or unusual bumps, which can indicate a cancerous tumor. The DRE can be a helpful supplement to prostate testing but is less accurate than the PSA test.
The PSA test checks your blood's levels of prostate-specific antigen, a protein produced by both cancerous and noncancerous tissue in the prostate. Normal levels are less than 4 nanograms per milliliter of blood, so higher levels can be a red flag for cancer. Importantly, though, several other conditions, such as an inflamed or enlarged prostate, could increase PSA levels and complicate the interpretation of the test results. Research has suggested about 70 percent of men with increased serum PSA levels did not have prostate cancer. However, the exams are important and the results will help guide your doctor to the next steps in assessing your health.
If the tests show nothing unusual, the doctor may recommend screening with one or both tests every one to two years.
What your results mean
Screening and follow-up testing can happen in a few different ways. If you begin with a DRE and your doctor finds an unusual lump or formation, they will proceed to check your blood PSA levels with a PSA test. If you begin with a PSA test and your levels come back high, they may perform a DRE. The two are complements. If both your DRE and your PSA test come back with abnormal findings, your doctor will discuss the next step, which will likely be a prostate biopsy.
In a DRE, an abnormal finding will be a lump or some other physical irregularity. Different professionals consider different PSA levels to be abnormal, but typically:
- Men with under 4 nanograms of PSA per milliliter of blood are unlikely to have prostate cancer.
- Men with between 4 and 10 nanograms per milliliter have a 1 in 4 chance of having cancer.
- Men with more than 10 nanograms per milliliter have a 50 percent chance of having cancer.
If your results come back in these ranges, in some cases, your doctor may only ask you to wait and have your PSA levels tested again later. However, if your doctor strongly suspects you're at risk of prostate cancer, they may order a biopsy.
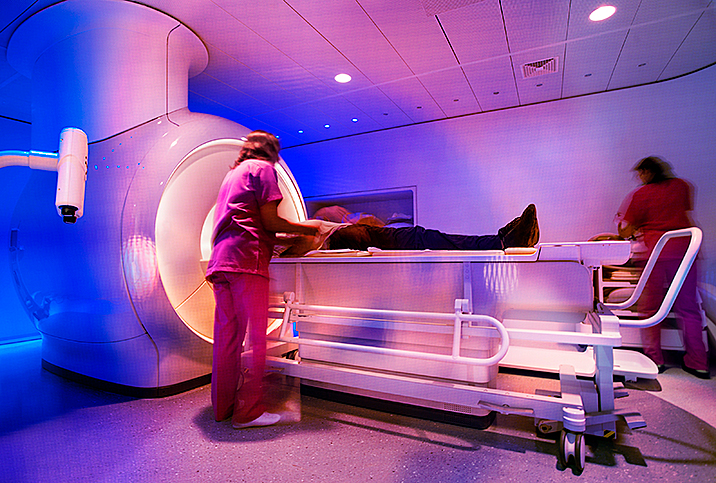
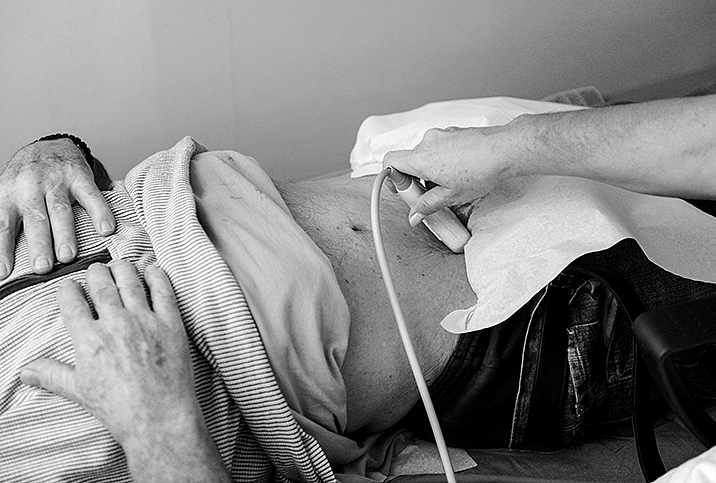
Typically, for the prostate, a urologist will perform a core needle biopsy. First, they will examine the prostate through an ultrasound or an MRI or a combination of both. Then, they will insert a spring-loaded hollow needle into the prostate, either through the rectum or perineum, and extract a "core" of prostate tissue. They typically do this 12 times. It's not nearly as painful as it may sound, and many doctors use an anesthetic before the procedure. You'll probably take antibiotics afterward to prevent infection, and you may experience soreness and blood in your urine and semen.
Your results will come back in a few days as either positive for cancer, negative for cancer or suspicious. In the case of a suspicious result, you may repeat previous tests or get another biopsy.
It might not be cancer
As mentioned, the PSA levels in your blood and the findings of your DRE can be altered by conditions other than cancer. This does not necessarily make the exams less useful; rather, think of this as an opportunity to get to know your all-around prostate health better. Commonly, a prostate exam may detect an inflamed or enlarged prostate—prostatitis and BPH, respectively.
Prostatitis typically causes pain or a burning sensation while urinating, as well as issues with the urination stream, such as hesitation, frequency or dribbling. Note the condition of the urine, which might appear bloody or have traces of blood. Nocturia, which is excessive urination during the night, may also occur. Prostatitis may cause men to experience pain in the groin, pelvic or genital area, and potentially the lower back and abdomen.
Benign prostatic hyperplasia is a nonmalignant enlargement of the prostate gland that occurs when the gland's cells start to multiply and cause swelling that interferes with urine flow.
If you're undergoing a prostate exam, it's important to tell your doctor if you've experienced any of these symptoms, as it may prevent any undue worry or unnecessary testing should your initial screenings come back abnormal.
When to get an exam
Because current prostate screening tests are not wholly accurate and come with a risk of both over- and underdiagnosis, the American Cancer Society recommends men have a thorough conversation with their doctor and engage in shared decision making. No prostate screening tests should be performed until the patient is fully informed of their limitations and benefits. This conversation is recommended for men at different ages, depending on a variety of factors.
If more than one close, or first-degree, relative has been diagnosed with prostate cancer at an early age, you should begin screening at 40 years old. If you are Black or have a close relative (father or a brother) who was diagnosed with prostate cancer before age 65, you should begin screening at 45 years old.
If none of the factors apply to you and you are expected to live at least 10 more years, begin screening at age 50.