Magnetic Resonance Imaging Gains Integration in Prostate Exam Process
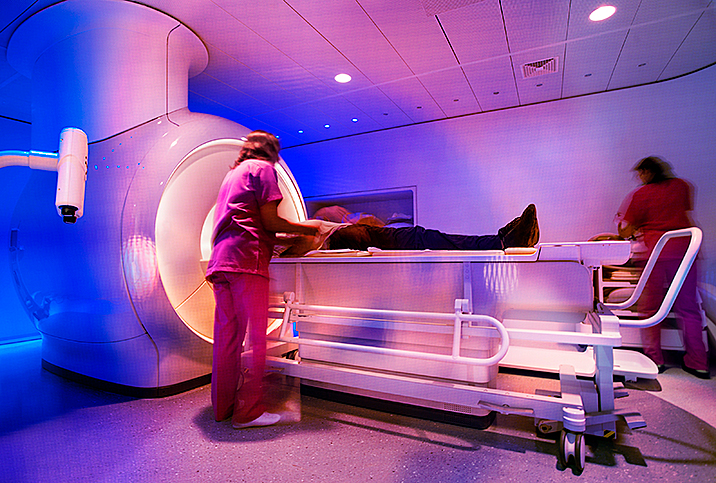
You used to go for a prostate exam, and if doctors had concerns about the findings of the digital rectal exam (DRE) and/or the prostate-specific antigen (PSA) blood screening, they might send you for a biopsy to see precisely what was going on.
Today, magnetic resonance imaging (MRI) is increasingly being used as a tool either before or after biopsies to determine whether a man has prostate cancer.
"It's definitely come in the mainstream and it's a really popular tool right now," said Christopher Russell, M.D., a urologist with AdventHealth Medical Group in Orlando. "The MRI is kind of our best tool for looking in the pelvic area."
When do doctors use MRI in prostate screening?
There are two instances when doctors may use an MRI to screen for prostate cancer, said Brian Keith McNeil, M.D., chief of urology at the University Hospital of Brooklyn and associate dean for clinical affairs at SUNY Downstate Health Sciences University in Brooklyn, New York.
"MRI [offers] optimized detection of clinically significant prostate cancer in men who we think may have prostate cancer who [haven't had a biopsy], or who have had a prior negative biopsy," McNeil said.
In the first scenario, the MRI is an intermediate step between a prostate exam, such as a DRE or PSA test, and a biopsy.
"Before doing a biopsy, you want to know if there's something there that's significant," McNeil said. "In the prebiopsy setting, you can do an MRI to see if there's something there that looks suspicious."
Once conducted, the MRI is read and scored on what is called the PI-RADS scale, a 1 to 5 rating from low to high concern. PI-RADS stands for prostate imaging-reporting and data system.
The second scenario for using magnetic resonance imaging to screen for prostate cancer occurs when a patient has had a previous negative biopsy but their PSA levels continue to rise. PSA is a protein produced by both cancerous and noncancerous cells in the prostate gland. Elevated levels in the blood may indicate the presence of cancer, though not necessarily, because many factors can raise PSA levels. A biopsy detects cancer only in the area of the prostate from which tissue is removed, not the entire prostate, so an MRI can help doctors get a clearer picture of the situation.
"The MRI will help tell us whether or not there's something that maybe we missed [in the biopsy], or if there's something that we need to specifically target," McNeil said.
How helpful are MRIs in detecting prostate cancer?
Two clinical trials, PRECISION and PROMIS, have shown that MRI is very effective at detecting prostate cancer, Russell said. The PRECISION trial, for instance, showed a nearly 50 percent increase in the detection of high-risk cancer with MRI-targeted biopsies than through standard biopsies (95 men compared with 64), and about 58 percent fewer participants received a diagnosis of clinically insignificant cancer between the same two testing groups (23 men versus 55). Low-risk cancers typically are monitored and not treated, Russell said.
MRI has become more widely used for prostate purposes in recent years for three reasons:
- The technology has advanced.
- The cost of having an MRI has gone down, though it is still high.
- Medical professionals have gotten better at reading MRI results.
Still, magnetic resonance imaging alone won't tell you if you have prostate cancer—only a biopsy can do that.
What is the downside to MRI?
While MRI is an increasingly valuable tool for doctors in their efforts to diagnose and treat prostate cancer, the scans do have a couple of downsides.
"The issue now is that MRIs are just so expensive," Russell said, estimating that the cost of a DRE is the cost of a doctor's visit, a PSA panel is about $75 and an MRI is about $7,000. Still, an MRI is much less expensive than it used to be.
Additionally, an MRI can take 30 minutes or more, and the tight confines of the MRI tube can make some patients feel uncomfortable, McNeil said. An open MRI is less confining but may not be available for all procedures, and not all doctors or patients have access to them.
Next-generation scans
Even while magnetic resonance imaging is growing in popularity, its successor may be in the works. Russell said MRI may be obsolete for prostate cancer screening in the next five years, negated by PSMA PET-CT scans. The acronym stands for prostate-specific membrane antigen; positron emission tomography and computed tomography.
"They just got FDA-approved, but they're very, very sensitive and specific," Russell said of the scans.
He added that the tests are still very expensive and not yet widely used, but they are so effective that they may alter the entire prostate cancer screening process.
"In the academic community, there's some argument that at some point we may be able to treat based on just PSMA alone because it's so specific," Russell said. "The world of prostate cancer has changed exponentially in the last 10 years."