What Happens When Your IUD Falls Out?

Years of birth control trial and error eroded my trust in reproductive health. When I was fitted with an intrauterine device (IUD), I thought a savior had finally arrived.
And then my IUD fell out.
IUDs, also known as contraceptive coils, have often been hailed as a sign of reproductive progress, especially for people with vaginas whose options have been limited to pills with a grocery list of life-altering side effects.
Recommended by the American College of Obstetricians and Gynecologists (ACOG) as a "first-line" contraceptive, IUDs were selected by approximately 14 percent of women ages 15 to 44 using contraceptives from 2015 to 2017, according to the Kaiser Family Foundation.
Five months after insertion and immediately after sex with my partner, he discovered a graze on his penis and exclaimed, "I think your coil fell out." What followed was a blur of panic, confusion and a lot of unanswered questions.
How does an IUD work?
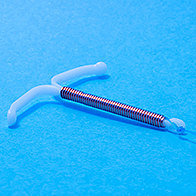
"There are two types of coil," said Nitu Bajekal, M.D., an OB-GYN in the United Kingdom and co-author of "Living PCOS Free." "One is a small T-shaped plastic and copper device with no hormones, known as a copper coil or intrauterine device or IUCD [intrauterine contraceptive device], and the other is a hormone-containing coil or intrauterine system [IUS]."
The IUS devices approved in the United States—Mirena, Kyleena, Liletta and Skyla—release small amounts of the hormone progestin into the uterus, making it more difficult for sperm to fertilize the egg and for an egg to implant. Mirena and Kyleena prevent pregnancy for up to five years, and Skyla and Liletta work for up to three years.
Despite being celebrated as an alternative to birth control pills, hormonal IUDs have similar side effects, including headaches, nausea, mood changes, breast tenderness and soreness, weight gain and acne.
ParaGard is the only copper coil in the U.S. approved by the Food and Drug Administration. Wrapped in fine copper wire, the IUD changes the cervical mucus, preventing a fertilized egg from implanting. It's one of the most effective forms of birth control with a one-year failure rate of around 0.8 percent.
The copper coil works as emergency contraception if inserted within five days of unprotected sex. Once in place, it works for up to 10 years. Side effects can include anemia, heavier bleeding and cramps, backaches, and pain during sex.
"I had chosen the copper coil because I had previously experienced side effects with two different versions of the pill," said Rachel Dalgarno, 35, an administrator with the U.K. National Health Service who had the coil inserted at age 33."I liked the idea of having something long term and not having to take any more medication."
IUDs are an attractive alternative to birth control pills thanks to their long shelf life, but the process of fitting them has been the subject of controversy. Medical websites and doctors alike frequently insist that the insertion process is "uncomfortable" at worst, however, some patients find it excruciating, and sedation is rarely offered.
The impact of IUD rejection and ejection
Motivated by a doctor's insistence that it would reduce my endometriosis symptoms, I had a Mirena IUS inserted as a quick fix for pain and birth control. Instead, it inflicted excruciating pain.
My doctor said there was a minor risk of rejection in the first two months. The IUS ejected itself from my body after five months.
"Coil ejection can happen but is uncommon, usually happening shortly after a coil has been fitted," Bajekal explained. "The cumulative risk of IUD expulsion is 10 percent over three years of use or 1 in 10."
A little frantic internet research later and I discovered that swift treatment was crucial. With the horrific side effects I had been experiencing, including the worst menstrual cramps of my life, I was surprisingly relieved to see the IUD expelled.
Dalgarno, whose coil was rejected shortly after she had it inserted, felt the same way.
"Three months after insertion, I noticed the strings were poking out more than normal and when I touched them, the coil fell out," she said. "I was actually relieved to see it and put its expulsion down to my body knowing what's best. Having a bit of plastic forcefully inserted into my uterus had clearly upset my body and it chose to reject it."
The precise reasons for IUD expulsion are unknown but may include incorrect positioning or a slightly opened cervix. Statistics show IUD expulsion occurs in 3 percent to 5 percent of all IUD users and 5 percent to 22 percent of adolescent IUD users, according to ACOG.
"The insertion feels like a trauma," Dalgarno said. "It was very painful, and no information I was given prepared me for the experience that I ended up having. Seeing the doctor after the expulsion felt like a waste of time, to be honest."
Knowing the risks of IUD rejection
As a sexual violence survivor, the process of IUD expulsion was particularly impactful for me. Undergoing any vaginal exam requires weeks of psychological preparation, but this experience required immediate treatment without my usual precautions.
While I am now confident that my new copper IUD will remain in place for the foreseeable future, the immediate aftermath left me in an unstable headspace.
"Most people will find this situation disappointing, frustrating and potentially embarrassing," said Charlotte Russell, a clinical psychologist living in Manchester, England. "It can help to understand that with all medical procedures there are risks that most of the time outweigh the benefits. However, occasionally, things don't go as we hope despite everything being done correctly."
Alongside the physical trauma, the experience triggered fear around having sex. I countered this by taking a gradual approach to reimmersing myself and decentring penetrative sex for a short while.
"My advice would be to get back into sex as soon as you feel comfortable enough and as long as you can do so safely," Russell continued. "Talk to your partner beforehand and explain what you do and don't feel comfortable with so that both of you are clear and you don't feel any unwanted pressure."
Improve awareness
Going through an IUD insertion and expulsion, I was ill-equipped and uninformed. People need to know the risks of expulsion prior to insertion, among other information about their reproductive health.
"There also needs to be more awareness raised about how having a coil can affect your periods and that expulsion can happen," Dalgarno said. "Better support should also be offered to women who experience significant changes or problems after insertion."