When is it Time to Schedule a Herpes Test?

There's a good chance you've never been tested for herpes, one of the most common sexually transmitted infections (STIs). While there are recommendations about routine screening for other STIs—for instance, all sexually active women should get tested for chlamydia and gonorrhea each year—there’s no such consensus surrounding testing for herpes. So, what gives?
Without clear rules, it can be confusing to know if and when you need to get tested. Even medical professionals can't always agree on when people should get tested.
The Centers for Disease Control and Prevention (CDC) estimates that one out of every six people ages 14 to 49 has genital herpes. That’s a lot of people, but most will never know they have the virus because they have few if any very mild symptoms that they don’t notice. Adding herpes to routine STI testing may help clue in a lot of people to the infection, but experts disagree whether this is necessary—and some argue it might be harmful.
“We haven't fully wrapped our heads around how widely to cast the herpes testing net," said Fred Wyand, director of communications at the American Sexual Health Association in Durham, North Carolina. "There's still a lot of stigma around herpes and treatment is of limited value in people who don't have symptoms. Testing everyone might cause unnecessary distress. Of course, the counter to that is people might be more likely to practice safer sex and have sexual health discussions with new partners.”
H. Hunter Handsfield, a medical doctor and professor emeritus at the University of Washington, added that the only way to test for herpes when there are no symptoms is by drawing blood, which can often give misleading results. Blood tests for herpes, he explained, are most valuable under two circumstances—if someone has no symptoms but has a regular partner who has herpes or when a person has symptoms but results are inconclusive and that person can't undergo other types of tests (due to healing lesions that can not be swabbed). "These are the biggies," he said. Many doctors will also test pregnant women even if they don’t have symptoms because an active herpes outbreak during delivery can be dangerous to the baby.
One out of every six people ages 14 to 49 has genital herpes.
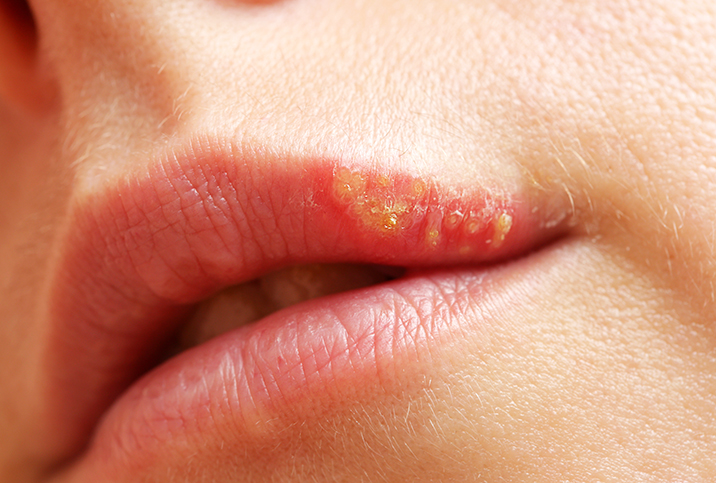
The best time to test for herpes is when you have symptoms, which usually start as a cluster of fluid-filled blisters near the site of infection—the genitals, mouth or anus. The blisters may itch or hurt. Eventually, they pop and become open sores, which can be painful, especially when they rub against your underwear or come into contact with urine. Some people get only one herpes outbreak in their life, while others have them every few months or years.
Your healthcare providers can swab the sores to determine whether you have herpes, and they can also determine which type of the virus you have. (This can help you know whether to expect future outbreaks and help make treatment decisions.) Wyand explained that the sooner the better for testing because "if the lesions have begun to heal or if sampled during a recurrence (less virus present)," it can be harder to swab them and get a positive result.
Experts may keep debating widespread testing. But when making decisions and suspecting herpes, the guidelines are rather simple. Get checked right away if you have symptoms. There’s no cure for herpes, but there are medications that can clear up symptoms and help prevent future outbreaks. (You may also have a different, more easily treatable STI.) Consider getting tested if you have a current or recent partner who has herpes.
Remember that herpes is often not included in routine STI tests, but don’t be afraid to ask your healthcare providers for a test, even if you don’t fit into one of the mentioned categories. It’s very unlikely they’d say no (they technically work for you), and there is no stigma in taking charge of your sexual health.