The Facts About Women's Reproductive Health

Reproductive health can be defined as a state of complete physical, mental and social well-being, according to the World Health Organization, and not merely the absence of disease. This includes the ability to have safe and satisfying sexual relationships, as well as the ability to have children with the freedom to decide, if, when and how to do so. Optimal reproductive health plays a critical role in enabling women to enjoy life, remain healthy overall and be active in their communities.
The reproductive health needs of women change with their life stages and are impacted by factors such as menstruation, fertility, contraception, pregnancy, sexually transmitted infections and chronic health issues, such as endometriosis and menopause.
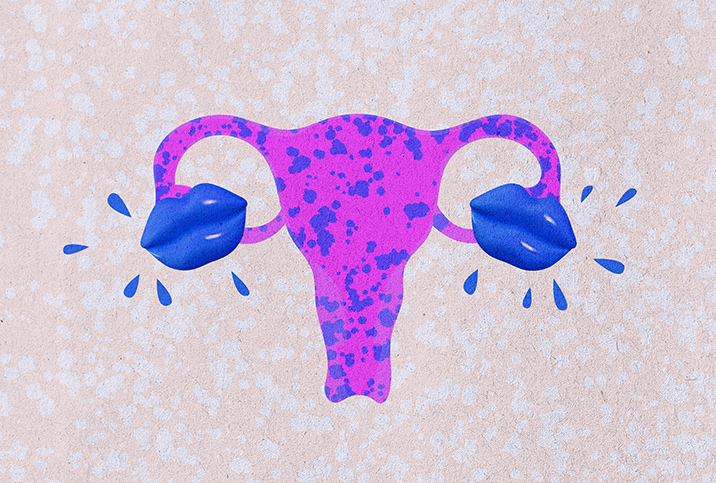
Welcome to the female reproductive system
Female sex organs consist of the breasts, cervix, ovaries, uterus and vagina, all working together to help a woman have children. This system is immature at birth, develops to maturity during puberty and then reduces its functionality during menopause in later life. The components' primary functions are:
- Breasts: These contain milk ducts and glands used for breastfeeding babies.
- Ovaries: Two small oval-shaped glands, the ovaries produce ova (eggs) and the sex hormones progesterone and estrogen.
- Uterus: A muscular organ, shaped like a pear, the uterus is home to a developing baby and is also known as the womb.
- Fallopian tubes: These narrow tubes extend from each side of the uterus to an ovary, carrying eggs from the ovary to the womb, where fertilization occurs.
- Vagina: A muscular canal, the vagina joins the cervix (the lower part of the womb) to the outside of the body.
Puberty is a phase during which a young female goes through biological or physical transformations, especially with respect to the reproductive organs. This process leads to sexual maturity and the ability to have children. Both genetic and environmental factors are involved in the timing of this important phase in a female's life, which usually begins between ages 10 and 14. Puberty causes physical changes such as breast development, hair growth in the pubic area and armpits, and, ultimately, menstruation.
Menstruation
Menstruation, or getting a period, is normal vaginal bleeding that occurs each month as part of the preparation process for a possible pregnancy. If no pregnancy occurs, the uterus sheds its lining, resulting in a period. The menstrual flow is partly blood and partly tissue from inside the uterus, passing out of the body through the vagina. This hormonal process usually starts at between 12 and 14 years old and continues until menopause at around 50 years old.
The menstrual cycle, which is counted from the first day of one period to the first day of the next, varies for every woman. Menstrual flow might occur every 21 to 35 days and last two to seven days.
Tracking your menstrual cycles can help you understand what your "normal" ovulation time is and identify important changes, such as a missed period or irregular, heavy or painful periods, which may signify health problems. Use a notebook, a calendar or a phone app to track your dates, flow rate and symptoms—especially if there's pain, unusual bleeding amount, mood changes and more.
A missed period can be an early sign of pregnancy.
Female sexuality
A woman's reproductive system is designed for the purposes of having children. For this to happen, a woman's egg must be fertilized by sperm, which usually occurs via sexual intercourse with a man, typically involving the insertion of the penis into the vagina.
Sexual health requires a positive and respectful approach to sexual relationships. This includes the prospect of having enjoyable and safe sexual experiences, free of intimidation, discrimination and violence.
Whether one views sex as a means to pleasure or in its biological role in procreation, sexuality is an essential part of everyone's personality. It is required for the survival of the human race, but on a more personal note, it's a basic need that enhances everyone's personal and social wellness.
Fertility, pregnancy and childbirth
Each month, one of a woman's two ovaries releases an egg in a process called ovulation. At the same time, hormonal changes prepare the uterus for pregnancy. If ovulation takes place and the egg is fertilized, it travels down the fallopian tube toward the uterus, where it will implant in the wall of the uterus, usually around four weeks after fertilization.
A pregnancy test is likely to give an accurate result if the woman takes it one week after the first day of the next expected period. Pregnancy tests work by analyzing urine for a hormone called human chorionic gonadotropin (hCG), which a woman's body produces only if she is pregnant.
Pregnancy usually lasts about 40 weeks, as measured from the last menstrual period to delivery. This is also called gestational age and is measured in weeks and divided into three segments called trimesters, or groupings, of 12 weeks.
A developing baby goes through important growth throughout pregnancy and is usually born spontaneously at between 37 and 42 weeks of pregnancy. Premature babies, those delivered anytime before 37 weeks of pregnancy, can have a higher risk of death and serious disability. As a result, clinicians keep a close eye on the number of weeks a woman is pregnant and how her cervix is preparing for delivery.
On the other end of the spectrum, some women have births that are delayed and need labor induction, a medical process that stimulates contractions of the uterus to trigger delivery. Methods of induction include both medication, such as prostaglandin, and physical approaches, like artificially breaking the water (amniotic fluid). Obstetricians—physicians trained specially in childbirth and the care of women giving birth—tend to induce labor only if there are major complications with the health of the woman or the baby, if the woman is several weeks past her full-term date or if it will reduce the risk of cesarean birth, preeclampsia and other health issues.
A cesarean section (C-section) is a surgical procedure carried out on a woman's abdomen to help deliver a baby when vaginal delivery might put the mother or the baby at risk. Although most C-sections are planned, some are undertaken due to unexpected problems during delivery, such as the size or position of the baby.
Contraception
Also known as birth control, contraceptives are methods to prevent pregnancy. A woman's choice of contraception depends on several factors, such as current health, frequency of sexual intercourse, number of sex partners and the desire to have children in the future.
Women can choose among several types of birth control:
- Barrier birth control prevents sperm from getting to the eggs. These include condoms, diaphragms, cervical caps and contraceptive sponges, and need to be used every time a woman has sexual intercourse.
- Natural rhythm calls for avoiding sex and/or using birth control only when the woman is most fertile, that is when—according to the calendar—she is most likely to get pregnant. An ovulation predictor kit or basal body temperature chart can be used to help a woman calculate her most fertile days.
- Short-acting hormonal birth control keeps a woman's ovaries from releasing eggs that could be fertilized. Types include birth control pills, patches, shots, vaginal rings and emergency contraceptive pills.
- Long-acting reversible hormonal devices are implanted into the uterus or upper arm by a physician and can be kept in place for several years. These include IUDs (intrauterine devices) and a newer long-acting reversible contraception that consists of an implantable hormonal rod placed in the upper arm.
- Sterilization, also known as female tubal ligation or occlusion, requires surgery and permanently prevents a woman from getting pregnant.
Menopause
Menopause is the time in a woman's life when she naturally stops having menstrual periods. Marking the end of a woman's reproductive years, menopause usually starts between the ages of 40 and 58 years, with an average age of 51 years.
At this point, the ovaries stop producing estrogen and other hormones, which has a ripple effect on the body, affecting sleep, mood, sexual function and more. Common symptoms include hot flashes, brain fog, mood swings, insomnia and vaginal dryness. Osteoporosis can also result, as the body starts to take in less calcium, causing bones to be more fragile and less dense.
While many women choose to treat their symptoms individually as they occur, some may decide to undergo hormone replacement therapy (HRT) to supplement the estrogen they've lost. Two common forms of HRT are systemic therapies and low-dose vaginal products. The former, taken as a pill, patch, gel or spray, circulates throughout the body and treats all menopausal symptoms. The latter remains localized, treating only vaginal and urinary menopausal symptoms.
Gynecologic health
Gynecology is the branch of medicine that specializes in women's health, especially as it relates to the reproductive system. A visit to the gynecologist is recommended for annual screenings and any time a woman has concerns about symptoms regarding her reproductive health. Many gynecologists are also obstetricians and are known by the shortened name OB-GYN.
Choosing a gynecologist that you feel comfortable with is one of the most important steps in maintaining your reproductive health. Make sure you do research and ask women you trust for recommendations. Reproductive health can impact your overall mental and physical health, as well as influence your self-image and relationships, so it's crucial to be diligent about gynecology appointments and find a doctor with whom you can freely communicate.