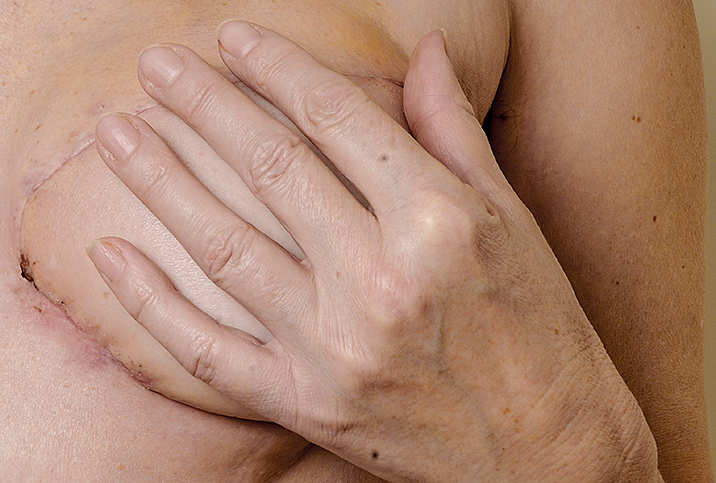
The Facts About Mastectomies

About 250,000 women are diagnosed with breast cancer each year, making it the second most prevalent cancer among U.S. women, according to the Centers for Disease Control and Prevention (CDC). In other words, a woman in the United States has about a 1 in 8 chance of developing invasive breast cancer over the course of her lifetime.
Fortunately, an increase in preventive healthcare has led to more early diagnoses and successful treatments, and the survival rates have improved over the years. While treatment for breast cancer can vary widely depending on the type and stage, most women undergo some kind of surgery along with their treatment program, according to the American Cancer Society.
The basics of mastectomy surgery
Before the surgery takes place, a surgeon or nurse will use a marker to draw lines around the breast to indicate where the incisions will be made. You'll then go under general anesthesia for the procedure.
The incisions the surgeon makes will depend on the type of mastectomy—skin-sparing, nipple-sparing and so on—but in any case, the breast tissue will be separated from the skin and muscle and removed. If you've opted for breast reconstruction in conjunction with your mastectomy, it's at this point your surgeon will perform that procedure.
At the tail end of the surgery, your surgeon will check for any bleeding and insert surgical drains. Then, they'll stitch and close the incisions, and wrap the surgery site in bandages. You'll be moved into a hospital room to recover. The length of stay averages three days.
Types of mastectomies
Breast-conserving surgery, called a lumpectomy, is a procedure in which a surgeon removes the cancerous cells and some surrounding healthy tissue but leaves the breast itself intact.
In cases where a mastectomy is necessary, however, the entire breast is removed. A mastectomy is typically performed when the cancer is too advanced for breast-conserving surgery to be effective, according to the Mayo Clinic. Mastectomy is an umbrella term for various types of procedures:
Simple (total) mastectomy
A procedure in which the surgeon removes the entire breast, including the nipple, areola and skin.
Double (bilateral) mastectomy
Resulting in the removal of both breasts, a double mastectomy is usually performed as a risk-reducing surgery for women who are at high risk for breast cancer due to a genetic mutation in the BRCA genes. In other cases, the procedure may be necessary as part of a breast cancer treatment plan. While a bilateral mastectomy typically entails removing both breasts entirely, in some cases, the nipples may be spared.
Skin-sparing mastectomy
This procedure involves the removal of the breast tissue, the nipple and the areola, but it spares most of the skin over the breast. Many women opt for this type of mastectomy because it leaves less scar tissue and preserves the opportunity for breast reconstruction surgery. A skin-sparing mastectomy may not be an option for an individual with a large tumor or one that is close to the skin's surface.
Nipple-sparing mastectomy
A version of the skin-sparing mastectomy, a nipple-sparing mastectomy involves removing the breast tissue while leaving both the skin and the nipple over the breast, but this option is only available when the breast tissue beneath the nipple and areola are free of cancer cells. While this surgery leaves fewer scars, the spared nipples may shrink or deform as a result of poor blood flow. This is considered to be an acceptable treatment for breast cancer but is usually recommended only for women with small or medium-sized breasts, according to the American Cancer Society.
Modified radical mastectomy
During this version of the surgery, the doctor performs a simple mastectomy and also removes the lymph nodes under the patient's arm.
Radical mastectomy
An extensive surgery that is rarely performed, a radical mastectomy includes the full removal of the breast and underarm lymph nodes as well as the pectoral muscles located under the breast. Though this surgery was once common, doctors have discovered less extensive surgery can be just as effective and cause fewer side effects.
Preventive mastectomies
Over the past couple of decades, more and more at-risk women have opted to get mastectomies before a cancer diagnosis, due to personal risk or concern. The rate of prophylactic (preventive) mastectomies more than tripled from 2002 to 2012, according to breastcancer.org. A woman might reach this decision because of a strong family history of breast cancer or if she learns she has a mutation on her BRCA1 or BRCA2 genes.
A prophylactic mastectomy can reduce breast cancer risk by 90 to 95 percent in women with the BRCA1 or BRCA2 mutation, as well as for women who have already had cancer in one breast and also have a family history of the disease, according to the Mayo Clinic. For these women, a prophylactic mastectomy may very well be an effective path forward. However, if a woman has no additional risk factors but has breast cancer in one breast, doctors have not found improved rates of survival for a prophylactic mastectomy of the unaffected breast.
Opting for a prophylactic mastectomy is a major decision. It's important to ask your doctor whether the procedure will change your risk of breast cancer significantly enough to warrant it. Ask about all of the prevention strategies available to you and be sure to get a second opinion before moving forward.
Postmastectomy side effects
Doctors usually recommend patients take it easy in the weeks following a mastectomy to ensure a full recovery. After about a month, most patients are able to return to regular activities.
Before you undergo a mastectomy, it's useful to be aware of some of the side effects you might experience after the surgery:
- Pain, tenderness or swelling at the surgery site
- Hematoma, or the accumulation of blood in the wound
- Seroma, or the buildup of clear fluid in the wound
- Limited arm and shoulder mobility
- Chest or upper arm numbness
- Nerve pain in the chest wall, underarm and/or arm that doesn't go away over time
- Lymphedema, if underarm lymph nodes are removed (lymph fluid in the fatty tissues builds up beneath the skin and causes swelling)
During a mastectomy, the breast nerves that transmit feeling from the breast and nipple are severed, meaning a woman loses sensation in her breasts, even after reconstruction. Nerves regenerate slowly, and a degree of sensation may not return for months. When sensation does return, it may never feel like it did before the procedure, a condition called postmastectomy syndrome.
Incisions from a mastectomy may take up to three weeks to heal, but there will be bruising and swollen areas for several months. Mastectomy scars may take months or several years to fade, and they will never disappear completely.
It's important to discuss with your doctor the symptoms of infection so you can seek help for anything out of the ordinary after surgery.
Best aftercare practices
Before you leave the hospital, make sure you know the steps to take at home before your first follow-up visit with your care team. Tasks that are likely to fall to you include emptying the drain bulb attached to your surgical drain and exercising the arm on the side of the surgery daily to prevent stiffness and soreness.
Until your drains and sutures are removed and your doctor clears you to shower, you'll need to take sponge baths. You may feel fatigue or pain that impedes your daily functions—don't try to "power through." Take pain medication if necessary, get plenty of rest and reach out to others for help with daily chores.
The road to recovery
Whether a woman gets breast reconstruction surgery following a mastectomy or not, she will likely go through issues with self-esteem and intimacy, and that is normal. Be sure to lean on your support system—partner, friends, family, therapist or support group—so you can successfully continue on your road to recovery.