Breast Procedures: Myths & Misconceptions
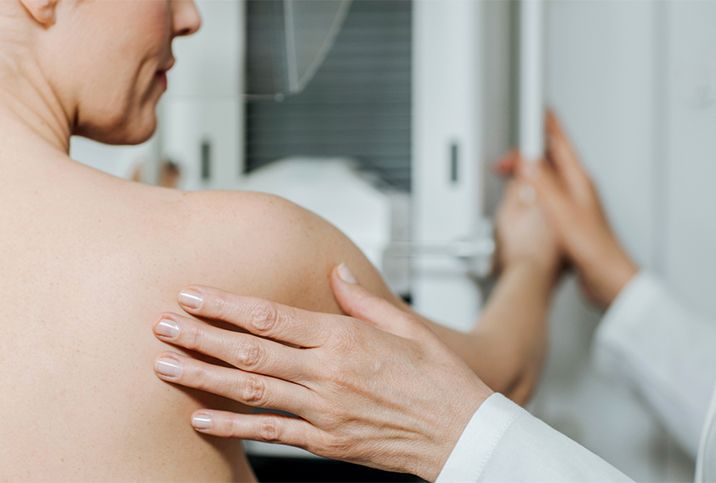
Procedures related to breast health and care range from the diagnostic, such as mammograms, to the cosmetic, such as breast augmentation, but also includes mastectomies and reconstructive surgery. All of these procedures can play a role in breast health, but misinformation about them abounds. Below, we set the record straight on a few of the most common procedures.
Mammograms
Most medical organizations agree that women can choose to begin getting regular mammograms& at age 40, but their actual recommendations for when mammograms should start vary widely.
The American Cancer Society advises women with an average risk to begin annual screening mammograms at age 45 until age 54, and then continue every two years.
Alternatively, the U.S. Preventive Services Task Force recommends women start screening every two years from age 50 until age 74.
The Centers for Disease Control and Prevention (CDC) has a handy chart with recommendations from across the healthcare spectrum.
Myth: I don’t need a mammogram if I don’t have any symptoms or a family history of breast cancer.
Reality: More than 75 percent of women who get breast cancer have no family history of the disease. It’s true that women with a family history of breast cancer are at an increased risk, but it’s important to remember that simply being a woman and getting older presents some risk of breast cancer. Therefore, mammograms are an important preventive health tool.
Myth: If my last mammogram was normal, it’s not a big deal to skip my next one.
Reality: Just because your last mammogram came back normal does not mean you don’t need another one in the future. Mammography acts only as a tool for detection, not prevention. Mammograms don’t prevent you from getting breast cancer, but they’re useful because they allow your doctor an opportunity to catch potential signs of cancer at the earliest possible stage, which gives you a better chance of successful treatment. Your body can change a lot in a year. So if you’re thinking about skipping your next mammogram, reconsider. That next one could very well save your life.
Myth: If I have breast cancer, a mammogram will always detect it.
Reality: While the value and importance of getting an annual mammogram once you turn the appropriate age cannot be overstated, the screening tool may not always detect cancer. In most cases, a mammogram will only miss signs of cancer in women with particularly dense breast tissue, although there are instances when even normal breast tissue can hide cancer. Despite that shortcoming, the annual mammogram has been shown to be an effective tool that has a net benefit for women’s health. Women under the age of 30 who require breast cancer screening should get an ultrasound, because they may have more dense tissue, whereas women over 30 should get a mammogram.
Myth: I should only get a mammogram if my doctor tells me to.
Reality: Doctors are human, too, and sometimes forget things—namely, reminding you to get your annual mammogram. If you are at least 45 years old (and younger if you’re particularly at risk), it’s important to be proactive about scheduling your mammograms. If you think you’re due for a screening and your doctor hasn’t mentioned it yet, bring it up during your next visit. Luckily, mammograms don’t always require a prescription, so it’s usually only a matter of making a couple of phone calls to schedule an appointment.
While deciding whether or not to get regular mammograms is ultimately a personal choice, it’s important to not allow misconceptions to keep you from receiving preventive care. The American Cancer Society reports that a woman in the United States has a 13 percent chance of developing breast cancer at some point in her lifetime. For this reason, maintaining regular preventive health checkups to screen for the disease could be lifesaving, as early detection increases the chances of successful treatment.
Breast Enhancement Surgery
Breast enhancement surgery—also known as breast augmentation—has remained the top cosmetic surgical procedure in the United States since 2006. Despite its popularity, there are several myths and misconceptions surrounding breast augmentation that make many women wary and unsure about the safety and benefits associated with this procedure.
Myth: I won't be able to breastfeed.
Reality: Some women worry they won't be able to breastfeed after getting implants, but breastfeeding is generally not affected by enhancement surgery. The American Society of Plastic Surgeons recommends telling your surgeon if you plan to become pregnant and breastfeed, so they can adjust their surgical technique to provide a better outcome for the patient's goal of breastfeeding.
For example, your surgeon may suggest locating the implants under the pectoral muscle as opposed to over the muscle, and make incisions under the breast or armpit as opposed to around the nipple to minimize the surgery's effects on breastfeeding.
Myth: Recovery is very long and painful.
Reality: Recovery from breast enhancement surgery usually lasts no more than eight weeks; however, any pain you feel will likely dissipate significantly after the first week. During the first week, your surgeon may advise you to relax at home and take it easy, and resume light activities at the beginning of the second week. Any pain you experience during that time can usually be managed with over-the-counter pain relievers.
Starting from week two onward, your pain will start to go away and you can gradually resume normal activities as advised by your surgeon and while monitoring your symptoms closely.
Myth: Implants will last a lifetime.
Reality: Most manufacturers of breast implants recommend having them replaced or removed every 10 to 15 years, although some surgeons may recommend leaving them in longer if the implants haven't ruptured, still look realistic and you're satisfied with their performance and appearance.
Your surgeon will explain the various signs and symptoms to watch out for that may indicate you need your implants replaced or removed based on the type you have.
Myth: Saline is safer than silicone.
Reality: Many women believe saline implants are safer than silicone implants because, if the implants should rupture and leak, silicone is not safely absorbed by the body like saline.
The truth of the matter is that silicone implants are less likely to rupture than saline implants, with research showing that 1.1 percent of silicone implants rupture within six years and 16 percent of saline implants rupture within seven years. Each implant type has its own pros and cons, which is why plastic and cosmetic surgeons will talk with you at length about your options before you make a final decision.
Medical advances have come a long way since breast implants first became available in the early 1960s. Today, breast implants come with very few health risks when enhancement surgery is performed by an experienced, board-certified surgeon. Ask your physician for more information if you are interested in getting breast enhancement surgery.
If you've already had breast augmentation, remember that regular mammogram screenings are still very important for your health. Always talk to your doctor about any questions or changes in your health as related to breast tissue.
Breast Reduction Surgery
Breast reduction surgery offers a variety of benefits for women who want to reduce the burden and discomfort associated with large breasts. Unfortunately, myths about the procedure often prevent women from undertaking this helpful cosmetic treatment.
Myth: I must wait until I'm done having children to get the surgery.
Reality: You can have breast reduction surgery at any time in your life, regardless of whether you're planning to have more children. Often, cosmetic surgeons recommend waiting until you're done having children only because pregnancy can cause your breasts to expand and grow larger to accommodate your baby's milk supply. Pregnancy after breast reduction surgery may negate the results of the procedure, but you don't necessarily have to wait until later in life to have it done. If you want breast reduction surgery but also want to leave your options open in terms of pregnancy, talk to your surgeon about the pros and cons of having surgery.
Myth: I can't breastfeed after reduction surgery.
Reality: Women can certainly breastfeed after breast reduction surgery, as long as their surgeon takes care to preserve the lactating part of the gland under the areola, known as the column of subareolar parenchyma. In a 2017 study published in PLoS One, researchers set out to determine whether breast reduction surgery impacted breastfeeding success. They found that women whose surgeons fully preserved the column of subareolar parenchyma experienced 100 percent breastfeeding success, while women whose surgeons partially preserved this part of the gland experienced a 75 percent success rate. If you plan to breastfeed in the future, inform your surgeon, who can then use proper surgical techniques to preserve lactating breast tissue.
Myth: Reduction surgery will leave me with noticeable scars.
Reality: While some scarring is unavoidable, most surgeons will use techniques to make scarring less noticeable. In addition, they should provide you with useful postoperative instructions that can help minimize scarring, such as wearing a compression garment for several weeks. Other steps you can take to minimize the appearance of scarring after breast reduction surgery include performing scar massage, wearing sunscreen, applying scar gels and undergoing fractional laser treatment. You should still discuss these strategies with your surgeon before moving forward as everyone’s surgery and healing will vary slightly. Over time, though, your scars will gradually fade.
Myth: Reduction surgery cannot be covered by insurance.
Reality: Most health insurance plans will not cover cosmetic treatments such as tummy tucks or breast enhancements, for example. But they may cover breast reduction surgery if the procedure is deemed medically necessary to improve or prevent health problems. For instance, large and heavy breasts often cause back and shoulder pain, poor posture and spinal curvature, and fungi, rash or other skin problems can develop in the folds under the breasts. Contact your health insurance provider directly to learn more about your benefits and the steps you need to take to get breast-reduction surgery covered by your plan.
Breast reduction surgery can improve your quality of life if you have large breasts that are causing you pain or discomfort, are difficult to manage, or if you simply want to improve your proportions and overall appearance. Ask your primary care physician to refer you to a board-certified plastic or dedicated breast surgeon, and make sure you do your research. Many surgeons now do "cosmetics/aesthetics," and you want to make sure you have preservation of function for lactation, an especially important factor for the younger population.


















