Treatment of Breast Cancer

Worldwide, breast cancer is the most common cancer affecting women (except for nonmelanoma skin cancer). In America, 13 percent of women will be diagnosed with it in their lifetime. Age, exposure to hormone replacement therapy (HRT) and certain oral contraceptives, genetic mutations (such as BRCA1 and BRCA2), being overweight/obese, smoking, drinking too much alcohol, and a family or personal history of breast or ovarian cancer all increase a woman's risk. The good news is the mortality rate in the United States has dropped significantly since 2000, due in part to advancements in prevention, screening and detection, and treatments.
Potential treatments
Breast cancer treatments vary based on a number of factors: patient characteristics and preferences, involvement of genetic mutations, cancer grade (degree of abnormality of cancer cells) and, most important, cancer stage (0 through IV). Along with patient characteristics—previous breast cancer history and treatments, overall health, age, family history and genetic risk factors—staging is used to generate tailored treatment recommendations. Treatments for breast cancer commonly include surgery, chemotherapy, radiation, hormone therapy, targeted therapy, immunotherapy and palliative care.
Surgical treatment
A majority of women with breast cancer undergo some form of surgery, which can be used in an attempt to remove all cancerous cells, to explore the possible spread to the lymph nodes or to relieve the symptoms of advanced cancer. Reconstructive surgeries aim to reshape breasts after tissue is removed.
Surgeries can be either breast conserving (BCS), including lumpectomy, quadrantectomy or partial or segmental mastectomy, or more radical (mastectomy). In BCS, only the portion of the breast with cancerous tissue (plus a healthy margin as a buffer) is removed. During a mastectomy, the entire breast is removed, including, in some cases, the nipple, the lymph nodes under the armpit and chest muscles.
Women with early-stage breast cancer often have the option to choose between BCS and a mastectomy. BCS is typically followed by radiation treatment, whereas radiation is not always needed after a mastectomy. For women who are good candidates for BCS, its outcomes, in conjunction with radiation, are as good as those for women who get a mastectomy, with equivalent 20-year survival rates. In some cases, a mastectomy is recommended as the better option, particularly for high-risk women who have a larger tumor, a history of radiation treatment or have tested positive for the BRCA gene mutation. That said, a 2015 Clinical Medicine & Research study of more than 5,000 patients reported comparable survival rates between those who had BCS and mastectomy, and noted that women who received BCS followed by radiation had better outcomes than either form of surgery alone. Thus, both surgeries have good outcomes, which may be improved by an adjunct therapy.
Lymph node surgeries are also common to determine the stage and spread of cancer. A sentinel lymph node biopsy (SLNB) involves removal of only the lymph nodes most likely to be first affected, minimizing the side effects of lymph node removal, such as lymphedema (swelling). Axillary lymph node dissection (ALND) involves the removal of more lymph nodes, which provides a better picture but increases the risk of side effects.
Surgeries for advanced cancers can help decrease symptoms, reduce pain and slow the spread, although surgery alone rarely cures metastatic cancers. In these cases, surgery can close wounds and remove a metastatic tumor, such as one in the brain or near the spinal cord.
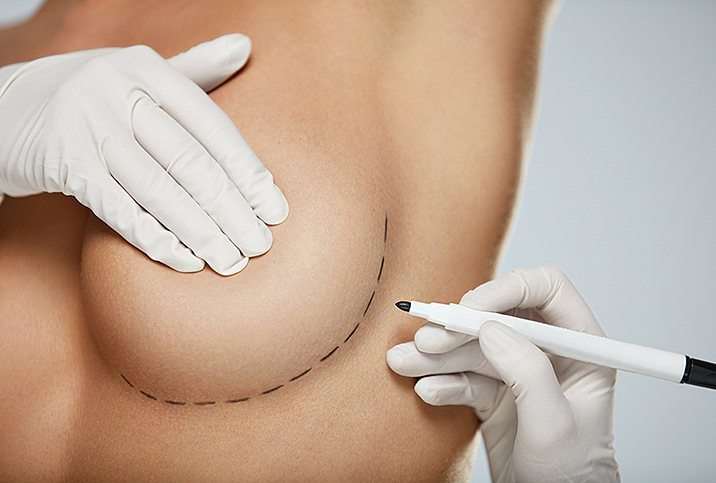
Breast reconstruction is an option that can be done concurrently with breast surgery or at a later time.
If you are recommended for surgery, meet with your breast surgeon (and plastic surgeon if you are undergoing reconstruction during the same procedure) to ask questions. Knowing what to expect can help you create an all-important patient support system. You'll review your entire medical history and medications list with the medical personnel, and they may recommend that you give blood, in case you need a transfusion during surgery. Other tests may be ordered, including a chest X-ray, an EKG, a CT and blood and urine tests.
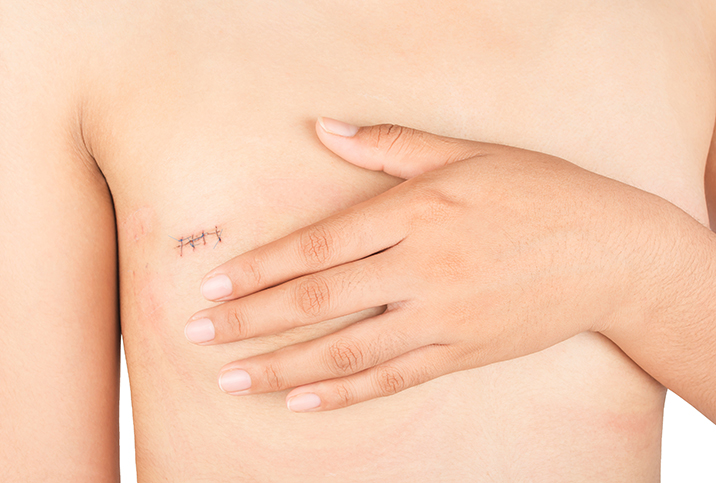
Any breast surgery can be an emotional challenge, so whether you're getting a BCS or a mastectomy, research the experiences of other women who have undergone them. BCS is usually performed on an outpatient basis, meaning you'll go home the same day. Mastectomy and ALND often require a one- or two-night stay in the hospital. You may go home with drains in your breast and armpit, to prevent fluid collection. Your doctor will explain how to manage the drains and care for the incisions and stitches, what exercises you can do to prevent stiffness and when you can wear a regular bra. Ask about a compression bra for use after surgery and a pain management plan. Depending on the type of surgery, most patients are back to normal activities in six to eight weeks.
Radiation treatment
Commonly paired with BCS or a mastectomy, radiation uses high-energy beams to treat breast cancer by killing cancer cells and helping prevent a recurrence. Radiation typically doesn't begin until the wound sites from surgery have healed and, in some cases, until after chemotherapy is completed. Prior to external beam radiation therapy (EBRT)—which is painless and lasts just a few minutes—technicians make small ink marks on your skin to mark target areas, and calculate angles for beams. Whole breast, chest wall and lymph node radiation are all typically conducted five days a week for six weeks. Short-term side effects may include fatigue, a sunburn-like rash on the treated area and breast swelling. (The side effects of brachytherapy, or internal radiation, are similar.)
After treatment, protect your skin from the sun and avoid lotions or perfumed products. Skin changes should abate in a few months. Radiation also has long-term implications: It may affect breast reconstruction options, and it can cause breastfeeding problems and occasionally nerve damage, swelling or weakened ribs.
Chemotherapy
Chemotherapy, the intravenous (IV) or oral administration of anticancer drugs, may be recommended after surgery (to kill any cancerous cells that were left behind and reduce the risk of recurrence), before surgery (to try to shrink the tumor and make for a less invasive or less extensive surgery), or in cases of advanced cancer that has spread beyond the breast and underarm region. Certain tests, such as Oncotype DX, help identify which women are good candidates. Typically, a combination of two to three chemotherapy drugs—anthracyclines, taxanes, 5-FU, cyclophosphamide and carboplatin—is used to maximize treatment effectiveness.
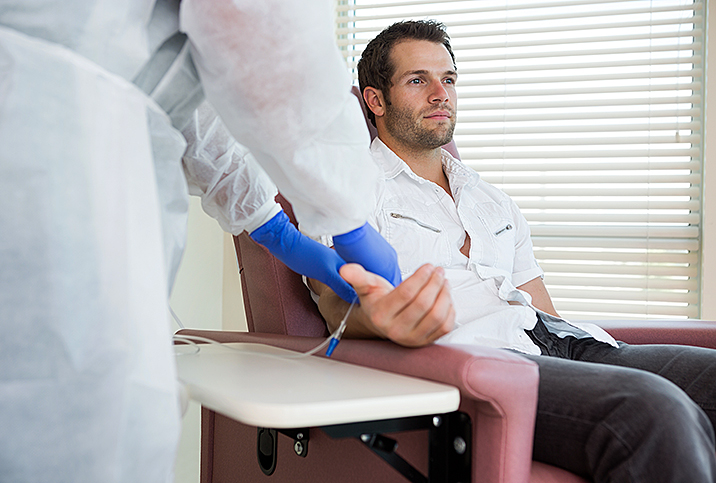
IV drugs can be administered over minutes or hours, typically in two- to three-week cycles, with break periods for recovery. Shortening the time between cycles and increasing the dose intensity, according to research from the Lancet, may increase the effectiveness of treatment and decrease the risk of recurrence. Total treatment is often three to six months but may be longer for cases where the disease is advanced. Administration of chemo drugs can be done at a hospital, a doctor's office or an infusion center.
Chemotherapy causes a number of dramatic side effects: hair loss, fatigue, nausea and vomiting, diarrhea, appetite and weight loss, mouth sores, nail changes, increased risk of infections, bruising and bleeding. The effects typically subside after treatment ends.
Menstruation and reproductive changes can also result from chemotherapy, including early menopause and infertility. While pregnancy is possible after chemotherapy—be sure to discuss fertility preservation options with your doctor—the drugs are not safe for a developing fetus (with the exception of a few drugs for women who are already pregnant when diagnosed). As a result, birth control is very important during this time. Early menopause caused by chemo can increase the risk for bone loss, so medications may be prescribed to help protect bone density.
Chemotherapy drugs can also cause heart and nerve problems, hand-foot syndrome and "chemo brain," which refers to slowed cognitive processing and issues with concentration and memory that may last for years after treatment.
Hormone treatment
Estrogen and progesterone receptor-positive breast cancers can be managed with hormone (or endocrine) treatments, which block cancer cells from attaching to the hormones and thereby stop them from growing. While only two out of three breast cancers are hormone receptor positive, candidates can benefit from this successful treatment, which reaches cancer cells almost anywhere in the body. It's typically used after surgery to reduce recurrence risk and is taken for five to 10 years, or to treat recurrent cases or metastasis.
Hormone therapies include selective estrogen receptor modulators (SERMs), either tamoxifen, toremifene or raloxifene. Side effects include hot flashes, vaginal dryness or discharge, and, very rarely, uterine cancer, blood clots, pulmonary embolism and stroke. The benefits outweigh the risks for most patients, and postmenopausal women benefit from the bone-strengthening effect of tamoxifen.
Another drug, fulvestrant, damages estrogen receptors and is given monthly by injection. It can cause hot flashes, headaches, nausea and bone pain. Aromatase inhibitors (AIs) lower estrogen levels by halting production and are primarily used in postmenopausal women. AIs are taken orally, once a day, alone or after tamoxifen, and can treat more-advanced hormone receptor-positive cancers. They can cause muscle and joint pain and stiffness, and osteoporosis. Finally, premenopausal women may take ovarian suppression drugs, like luteinizing hormone-releasing hormone (LHRH) analogs, to stop estrogen production in the ovaries. These may be used alone or in combination with tamoxifen, AIs or fulvestrant.
Palliative care
Improving your quality of life can be just as important as treating the disease. Palliative care relieves treatment side effects like pain and nausea, is helpful in advanced cases and end-of-life care, and even supports the bereaved. In addition to improving patient comfort, it provides resources for coping and counseling, and can help people make treatment and other care decisions and address spiritual and emotional concerns. Oncology teams, from clinicians to social workers and chaplains, typically provide palliative care, and it can play an immensely impactful role in ameliorating emotional and physical discomfort for the breast cancer patient and loved ones during a difficult time.
Palliative care needs a PR campaign, though. According to data from The New England Journal of Medicine, 70 percent of Americans don't know what palliative care is; even most physicians were found to equate it with end-of-life care. Ask about it if your oncology team doesn't bring it up with you first.
Recovery
Recovery from breast cancer varies based on the treatment and the treatment timeline. Women who undergo surgery typically recover in two to three weeks. If they receive radiation and/or chemotherapy, treatment timelines may be elongated to as long as six months or more. Hormonal therapies are ongoing and may last five years or longer.
Even after treatment ends, your body won't recover right away: It'll take time getting back to your normal energy levels, allowing scars to heal, healing sensitive skin from radiation and regrowing hair after chemotherapy. Breast cancer and its treatment do a number on the body. Taking care of yourself now is essential. Eat well, stay hydrated, get lots of rest, treat yourself regularly to a massage or a relaxing activity and give yourself the time to heal, physically and emotionally.
Create a support system and consider joining a formal support group. Millions of women (and thousands of men) can relate to what you're going through, and they may offer meaningful advice and words of support if you connect with them.
Outlook
Breast cancer treatments are extremely effective for the majority of cancers, and the likelihood of survival increases with earlier detection. The five-year survival rate for stage I breast cancer is 90 percent, meaning 9 out of 10 women are still alive five years after having been treated for stage I breast cancer. Those odds jump to 99 percent for invasive breast cancer contained within the breast. The 10-year survival rate for nonmetastatic invasive breast cancer is 84 percent.
Recurrence rates depend on multiple factors, including the individual, the type of cancer, its stage, treatments utilized and more, and the chances of a recurrence may range from 40 percent or greater to as low as just a couple percent. The risk of recurrence can be minimized through treatment methods such as radiation and hormone therapy and lifestyle change. Positive changes include stopping smoking, eating a healthy and balanced and predominantly plant-based diet, maintaining a healthy weight, minimizing alcohol consumption and avoiding exposure to environmental toxins. More recent developments in treatment have further improved options and outcomes for patients.
Breast cancer is a major life obstacle shared by the patient and an extensive circle of friends and loved ones. Today's medical treatment options, available support systems and known ways to help prevent the disease provide good reason for optimism.