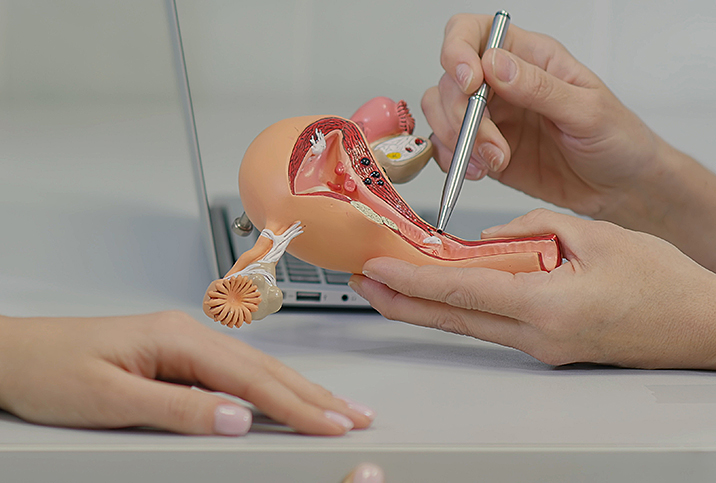
How Your Genetics Affects Your Risk for Ovarian Cancer
An estimated 21,410 women in the United States will be diagnosed with ovarian cancer in 2021, and about 13,770 will die of the disease, according to the American Cancer Society.
While ovarian cancer can occur in women of any age, it's most common among women between the ages of 50 and 60. Other factors that put an individual at greater risk of ovarian cancer include having a family history of the disease and undergoing estrogen hormone therapy. Women who either started their period at an early age or began menopause at a later age (or both) may also be at higher risk of developing ovarian cancer.
The link between DNA & ovarian cancer risk
Genetics can play a significant role in ovarian cancer risk.
According to the National Ovarian Cancer Coalition, more than 20 percent of ovarian carcinomas have been related to hereditary conditions. In fact, findings in the journal Molecular Oncology assert that half of all families with two or more incidences of ovarian cancer carry mutations of the BRCA1 or BRCA2 genes. It's also possible that sporadic gene mutations can lead to the development of ovarian cancer.
In general, an estimated 1 in 500 people have either the BRCA1 or BRCA2 mutation, or both. According to medical experts, certain women are more likely than others to have these mutations. For example, the BRCA1 and BRCA2 mutations are much more common among individuals of Ashkenazi Jewish descent, with an estimated 1 in 40 having one or both mutations.
Other genetic mutations that are known to increase a woman's risk for ovarian cancer include mutations associated with Lynch syndrome, which predisposes a patient to many forms of cancer, most notably colorectal but also ovarian.
It's important to note, though, that most ovarian cancers are not related to hereditary genetic mutations.
Assessing your risk
The only way to know for sure if you've inherited a predisposition to ovarian cancer is to get your genes tested. Talk to your doctor about whether your situation—being pregnant or having a significant family history of the disease, for example—qualifies you for help from your insurance carrier. Your doctor or a genetic counselor may be able to help you understand your test results.
To increase your chances of detecting and addressing abnormalities as soon as they arise, be sure to maintain regular preventive healthcare checkups and alert your doctor if you experience any persistent issues out of the ordinary or know of a family member recently diagnosed with a genetic condition. Ovarian cancer doesn't always cause symptoms, which can be general, but when it does, they can include bloating, pelvic or abdominal pain, nausea, constipation, sudden weight loss and a persistent and frequent urge to urinate.
If you're worried about your risk for ovarian cancer, talk to your doctor. As with many types of cancer, ovarian cancer may be treated more effectively with a better prognosis when it's detected early, so take precautionary steps to assess your risk and come up with a detection and prevention strategy that's right for you.