What is Mayer-Rokitansky-Küster-Hauser (MRKH) Syndrome?
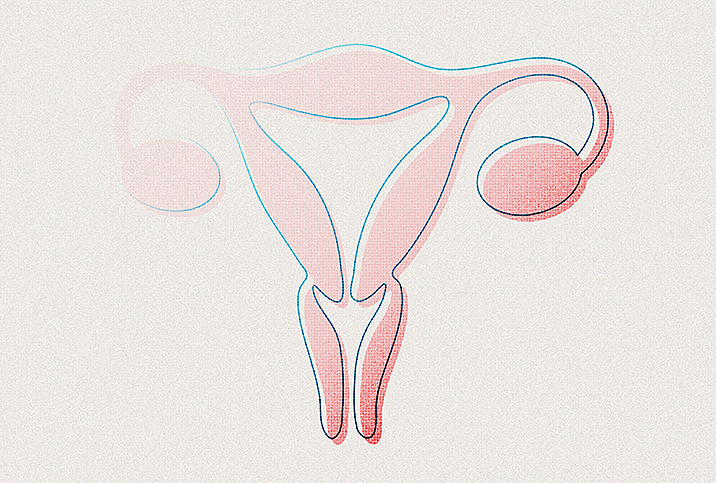
Mayer-Rokitansky-Küster-Hauser (MRKH) Syndrome is a congenital condition that affects approximately 1 in 4,500 women, though this statistic may not account for transgender men and non-binary people. This condition involves the underdevelopment of the reproductive tract in people assigned female at birth. However, the vulva presents normally.
Diagnosing MRKH
The underdevelopment or absence of a uterus, cervix or vagina means that people with MRKH don't menstruate. Mayer-Rokitansky-Küster-Hauser Syndrome is still widely unheard of, including in the medical community, and getting diagnosed can be difficult. I was lucky as a teen to live only an hour away from Boston, where I had access to the help and advice of one of the few MRKH specialist gynecologists in the United States at the time (2009).
Most people find out in their teenage years, when they have tests conducted, such as an MRI or pelvic ultrasound, to help doctors understand why they have not begun menstruation. In my case, I had both the pelvic ultrasound and the MRI, though not on the same day. I also didn't receive the results until a later date when we were able to set up an appointment with the local specialist.
There are two types of Mayer-Rokitansky-Küster-Hauser Syndrome. Type 1 is the most common. It is simply the absence or underdevelopment of the uterus, cervix and vagina. The ovaries are functional in most cases. Some people with Type 1 MRKH may have endometriosis. Type 2 is less common and may involve additional differences in the development of the kidneys (such as only one kidney), bone structure (such as osteoporosis or scoliosis), hearing faculties (ranging from tinnitus to deafness) and occasionally heart defects.
MRKH and mental health
A diagnosis of MRKH can severely affect mental health; some reactions are strong enough to be considered trauma. Often people with MRKH have feelings of loss, anger and grief. Society has trained women to obtain value from their ability to have children, which means this diagnosis can often lead to feelings of isolation and, as in any case of infertility, feelings of unworthiness. This diagnosis can lead people to question their gender and/or sexual identity and feel shame around having sex due to the need to explain potential issues to sexual partners. It is somewhat socially taboo to discuss matters of sexual health, even with potential sexual partners, though society accepts the importance of these conversations. Sexual intercourse can be physically painful due to the nature of the underdeveloped vagina, even after it has been lengthened. Anxiety and depression are common.
Treating MRKH
There are plenty of options for improving life after this diagnosis. One option is to have the vagina elongated through surgery. Another option is to use a dilator to elongate the vagina, which is less invasive than surgery.
As for raising children, world-over, adoption is still the only widely available option for infertile women, and often single women find it difficult to adopt. While surrogacy and in vitro fertilization (IVF) technologies have come a long way in the past several years, they are not yet legal in many countries, let alone possible. Research into uterus transplants has begun but remains in the trial process.
As for people with the second type of Mayer-Rokitansky-Küster-Hauser Syndrome, having smaller kidneys or only one does affect what types of activity doctors recommend, including what sports you should play, and diet has to be planned around your lack of kidney power. For instance, I only have one kidney, so I have a lower tolerance for alcohol than other women of my height and weight.
If you think you might have this condition or are worried about your physical or mental health for any reason, please speak to your doctor. MRKH can feel isolating, but it's important to remember you're not alone, and it's possible to live a happy, healthy life with this condition.















