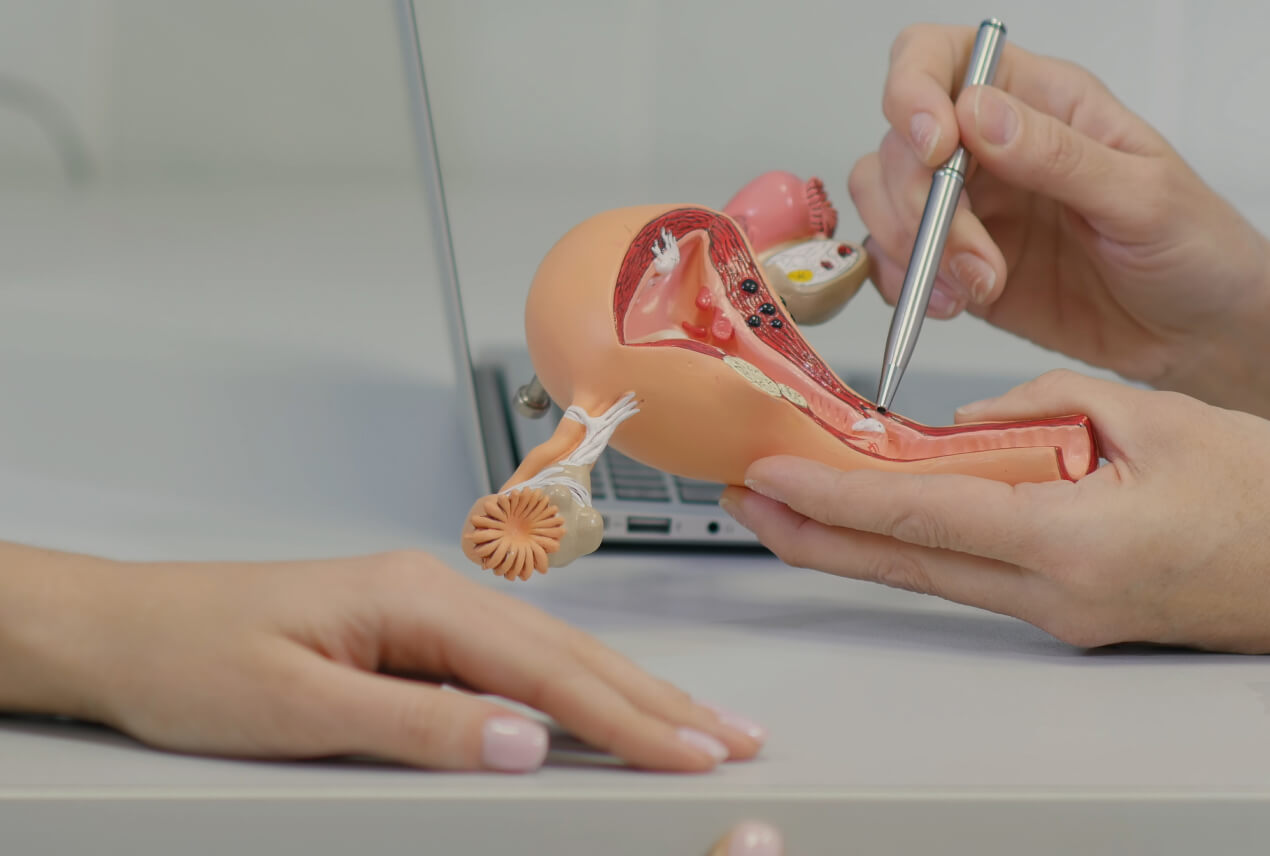
The womb is the part of a woman's reproductive system that holds and protects a baby during pregnancy. The endometrium is the lining of the womb, and endometrial cancer is cancer of the lining of the womb, or uterus.
According to the American Cancer Society, it is the most common cancer of the female reproductive organs. In the United States, there will be an estimated 65,950 new cases of endometrial cancers and uterine sarcomas in 2022.